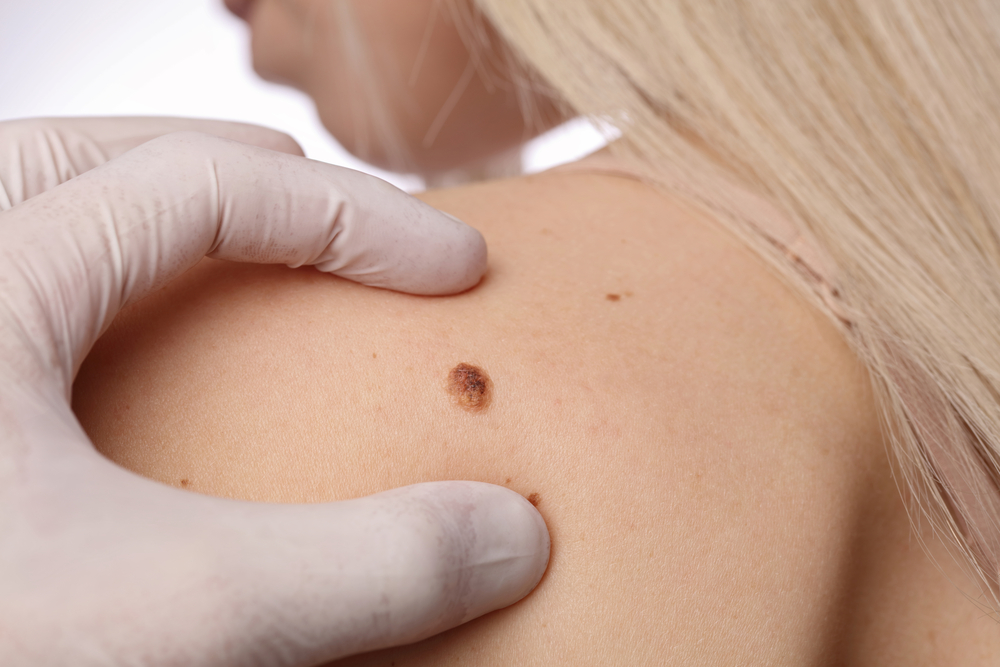
- Nearly 1 in 10 Americans have at least one precancerous mole.
- A precancerous condition refers to abnormal cells that are associated with an increased risk of developing cancer.
- Moles identified as precancerous may be removed via surgical excision.
Skin cancer is the most common cancer in the United States, with one in five Americans developing it at some point in their lifetime, according to the American Academy of Dermatology (AAD). A large number of Americans—about 33 million—also have precancerous moles.
What is a precancerous mole?
A precancerous mole refers to an atypical-looking (unusual or irregular) mole that has a greater chance of developing into skin cancer than a normal or common mole. Doctors refer to a precancerous mole as a dysplastic nevus (the pleural is nevi). Dysplasia means “containing abnormal cells” and nevus means “mole.”
Cells in dysplastic nevi behave abnormally, and are therefore referred to as precancerous. If the cells undergo further mutations, they may develop into cancer and spread to other areas of the body.
The good news is that the odds of a precancerous mole developing into cancer are really very low—many moles will remain nothing more than slightly odd-looking.
Precancerous cells are usually separated into different severities or grades of dysplasia: Low-grade dysplastic cells have a low risk of developing into cancer; high-grade dysplastic cells have a much greater risk.
What does a precancerous mole look like?
Normal moles are usually smaller than 5 mm wide. They are round or oval, have a smooth surface with a distinct border, and are uniform in color (usually pink, tan or brown).
In contrast, a precancerous mole has certain characteristics that are apparent to the naked eye. The National Cancer Institute (a division of the National Institutes of Health) describes a dysplastic nevus as appearing “flat with a smooth, slightly scaly or pebbly surface, with an irregular edge that may fade into the surrounding skin.” The institute also specifies that a dysplastic nevus may often be more than 6 mm wide.
According to the American Cancer Society (ACS), the signs to watch out for follow the mnemonic ABCDE:
- Asymmetry: One part of a mole does not match the other.
- Border: The edges are irregular, ragged, notched or blurred.
- Color: The color isn’t uniform and may include patches of brown, black, pink, red, white or blue.
- Diameter: The mole is larger than a pencil eraser (about 6 mm or ¼ inch), though some can be smaller.
- Evolving: The mole is changing in size, shape or color.
The ugly duckling (UD) sign is another way of identifying the possibility of skin cancer. It simply means that any mole or freckle that differs in shape, size or color from any other on the skin is often the most suspicious and therefore warrants further examination.
“Keep an eye on your body. Early detection is the key to fighting skin cancer. If you see a strange mole on your body, see a doctor right away,” says Dr. Bobby Buka, a board-certified dermatologist practicing in NYC. “Generally, dermatologists follow the ‘ugly duckling’ rule. Finding a mole on your body that looks different from the others is what a dermatologist will notice first.”
What’s the risk that a precancerous mole will develop into cancer?
It’s fairly common to have a precancerous mole. Approximately 1 in 10 Americans people have at least one dysplastic nevus. While a dysplastic nevus is more likely to develop into skin cancer, this outcome is by no means a given.
Dr. Jena Martin, a dermatopathologist practicing in Minnesota, notes that only about 20% of melanomas develop in moles that have been present since childhood.
However, the more precancerous moles an individual has, the greater their chances of developing melanoma. The chance of developing melanoma is about 10 times greater for someone with more than five dysplastic nevi than for someone who has none. People are also at greater risk if they have a relative who has developed melanoma or skin cancer.
“Once your dermatologist knows the pathologist has diagnosed an atypical mole on your skin, this tells the dermatologist that you are at a higher risk for developing a melanoma somewhere else on your skin,” explains Dr. Martin.
RELATED: Pediatric Melanoma — When to Worry About Suspicious Moles in Children
How often should I examine my precancerous moles?
People with dysplastic nevi—especially if they have several—should check their skin once a month, looking for the signs outlined above: changes in color, size, shape, texture, and surface, as well as itching or oozing. To help identify changes, you can take a picture of the moles each month and compare to past pictures.
People with more than five precancerous moles may want to have a skin cancer screening at a dermatologist’s office once or twice a year because of the moderately increased risk of skin cancer.
Individuals with a family history of melanoma may want to get examined more often— every three to six months. If your dermatologist thinks a mole appears suspicious, they may take a biopsy and send it to be tested.
“A skin biopsy can be performed by a professional in under five minutes. The procedure is practically painless and only leaves a tiny scar. After the mole is examined by a pathologist, it will be determined whether you’ll need additional removal,” Dr. Buka says.
Do precancerous moles need to be treated?
In general, dysplastic nevi do not need to be surgically removed because the risk of them developing into cancer is so limited. In fact, according to the American Osteopathic College of Dermatology, “Most of the melanomas found on people with atypical moles arise from normal skin and not an atypical mole.”
However, your doctor may recommend surgical removal of a precancerous mole if a biopsy is determined to be highly dysplastic, i.e., the mole is very likely to develop into cancer.
Your doctor may also recommend removal of a moderately dysplastic nevus if you have multiple atypical moles, if you have a family history of skin cancer or you have a history of cancerous moles.
How can I reduce my risk of developing skin cancer?
Whether you have precancerous moles or not, there are many practical steps you can take to prevent your risk of developing skin cancer. While certain risk factors—such as age, race, gender, and family history—can’t be controlled, you can manage other factors.
Sun exposure and the resulting damage to the skin from UV rays are known to increase the risk of developing skin cancer, especially people with multiple moles. It is important to avoid the sun—especially the most intense rays between 10 a.m. and 2 p.m. Wear UV-protective clothing, a hat, and sunglasses. Make sure you also wear plenty of broad-spectrum, water-resistant sunscreen, and reapply it according to the label’s instructions.
While precancerous moles are common, many never develop into skin cancer, and regular self-examinations can help identify any malignant changes and enable you to seek treatment quickly.
If you’re at risk for developing skin cancer, or have a dysplastic nevus that requires attention, meet our medical review team.