Finding an unusual spot on your skin can raise alarm bells. Noticing a small skin lesion that appears to be growing rapidly is an even greater cause for concern. While at first you may think that it’s a melanoma, you most likely have a more benign skin condition known as a keratoacanthoma.
First described in 1889 by English surgeon Sir Jonathan Hutchinson as a ‘crateriform ulcer of the face,’ the causes and nature of keratoacanthoma have been subject to much debate since. In fact, up until the 1990s only a dozen cases of mestastasizing keratoacanthomas had been properly recorded and studied.
More extensive research has been performed in recent years, and significant progress has been made in identifying and treating this relatively common skin condition.
To find out more, we consulted with two doctors who deal with keratoacanthomas in their clinical practices on a regular basis.
Dr. Todd Minars is Board-Certified Dermatologist and Assistant Clinical Professor of Dermatology at the University of Miami School of Medicine. His private practice is based in Hollywood, Florida.
Dr. Kachiu C. Lee is a Board-Certified Dermatologist and Assistant Professor of Dermatology at Brown University. She is also the Director of the Lifespan/LPG Laser and Aesthetic Center in East Providence, Rhodes Island.
What is keratoacanthoma?
Keratoacanthoma (KA) is a skin tumor most commonly found in elderly Caucasians. Its similarity in appearance with more aggressive forms of skin cancer often causes it to be misdiagnosed.
In fact, the diagnosis and categorization of KA is a controversial topic among dermatologist. Some studies suggest that it’s a form of squamous cell carcinoma (the second most common skin cancer after basal cell carcinoma), while others see it as a distinct entity with its own unique molecular signature.
According to Dr. Minars, keratoacanthoma is in fact a sub-type of squamous cell carcinoma. “It deserves its own sub-type because it often looks and behaves differently than a ‘real’ squamous cell carcinoma.”
Compared to a squamous cell carcinoma, a keratoacanthoma has the distinguishing feature of occurring in distinctive phases. “The first phase consists of rapid growth,” says Dr. Lee. “This is followed by a period of stabilization. The third and final phase is spontaneous resolution, although this does not occur in all cases.”
What causes keratoacanthomas?
For reasons that are still unclear to specialists, keratoacanthomas arise from hair follicle skin cells, most often on sun-exposed areas such as the head (face and ears), neck, and limbs.
Some studies suggest that keratoacanthoma may be linked to alterations in certain genes, while others point to a connection between the condition and human papilloma virus.
It has also been observed that trauma to the skin could potentially play a role in the development of keratoacanthomas. For example, they sometimes arise in people who have recently been tattooed. There is also speculation that they may be caused by contact with chemical carcinogens.
The general consensus is that keratoacanthoma is triggered by excessive exposure to the sun. As with skin cancer, ultraviolet light is thought to stimulate changes in skin cells that result in the formation of tumors.
What are the different types of keratoacanthoma?
There are two main types of keratoacanthoma, solitary and multiple, with several sub-classifications within these two types.
Solitary keratoacanthomas
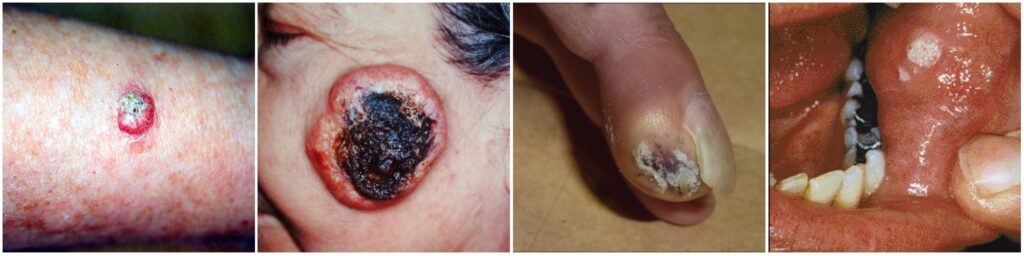
- Typical solitary keratoacanthomas can vary in their nature and appearance. What may first appear as a rose nodule can grow rapidly over a 3 to 6 week period to roughly three-quarters of an inch. It can remain in this mature phase for approximately 6 months before getting smaller and regressing entirely. These are commonly found on the arms and legs.
- Giant keratoacanthomas grow larger than three-quarters of an inch and predominantly appear on the eyelids or nose.
- Subungual keratoacanthomas are rarer, and appear under the nails.
- Mucosal keratoacanthomas are even rarer and appear intraorally, or in other words, in the mouth. Compared to other types of keratoacanthoma, a mucosal keratoacanthoma is less likely to regress.
Multiple keratoacanthomas
The classification of multiple KAs is not standardized, which often leads to confusion and overlapping. Several different types exist — some affect children, and others are more commonly found in elderly patients. Other types are found in patients of all ages. In either case, multiple keratoacanthomas are extremely rare.
“In fact, I have never seen this variant in my practice,” says Dr. Minars, “but I see solitary keratoacanthomas every day.”
Dr. Lee concurs. “Solitary lesions are the most common. Overall, people who have multiple keratoacanthomas are ones who have a suppressed immune system, inflammatory diseases, or other genetic conditions.”
How will you know if you have keratoacanthoma?
When a keratoacanthoma first appears, it may look like a pimple or a small boil. But when you try to squeeze it, you find it has a solid core that won’t pop the way a pimple normally would.
“Keratoacanthomas usually appear suddenly and grow quickly over the course of weeks into a volcano-shaped bump with a central crust,” informs Dr. Minars.
The central crust of a keratoacanthoma is a rapid growth of keratin, the protein produced by keratinocytes (skin cells). When keratin builds up, it produces scale, or dead skins cells. It’s this scale accumulation that causes the ensuing volcano-like eruption.
If you notice a spot on your skin that rapidly grows in size over a few weeks, do not delay in seeking the advice of a certified dermatologist for proper diagnosis and treatment.
Can anyone get a keratoacanthoma?
Keratoacanthoma can develop in anyone, at any age. However, since sun damage is the most likely cause, these growths tend to occur more frequently in older patients with overexposed skin.
Men may be more susceptible than women. Keratoacanthoma is less common in darker-skinned individuals.
Can keratoacanthoma become cancerous?
“Keratoacanthoma can become cancerous and also invade deeper skin structures such as nerves, a condition known as perineural invasion,” says Dr. Lee.
However, there is no need to be overly concerned. According to Dr. Minars, keratoacanthomas are the least common type of tumor to develop into skin cancer and generally remain benign.
However, dermatologists don’t have the tools to predict whether a keratoacanthoma will spontaneously resolve, or instead transform into a more aggressive tumor that affects the skin’s deeper layers. For this reason, keratoacanthomas should always undergo early treatment.
How do I know if I have keratoacanthoma or squamous cell carcinoma?
The following table outlines some of the key characteristic differences between the two types of tumors.
If you notice something unusual about your skin, it is always recommended to seek a proper diagnosis from a certified dermatologist.
| Keratoacanthoma | Squamous Cell Carcinoma |
|---|---|
| Rapid growth | Slow growth |
| Distinct edge between the tumor and stroma | Indistinct |
| Epithelial lip | No lip |
| Ulceration | No ulceration |
| Relatively rare | Common |
How do you treat keratoacanthoma?
Even though keratoacanthoma can self-heal, there is no reliable tool to determine the difference between a keratoacanthoma and a cancerous lesion. Therefore, keratoacanthomas require treatment by a certified dermatologist.
“Like any skin cancer we start with a shaved biopsy of the tumor,” informs Dr. Minars. This involves shaving off a portion of the lesion and sending it to the lab for analysis.
Interestingly, although the shave biopsy is not intended to be the treatment, it can often be curative.
“When I shave them off, I can often see the ‘core’ of the tumor, which looks like a little mushy ball in the dermis (skin) beneath the shaved-off top of the bump,” says Dr. Minars. “As long as I scrape out the core with a curette at the time of biopsy and lightly cauterize the base, the tumor is usually cured.”
“When the patient comes to their follow-up appointment, if there is any remaining keratoacanthoma, then a simple five-minute procedure is typically required and is generally curative. This procedure requires numbing the area, scraping it out, and lightly cauterizing it. Once in a while, a keratoacanthoma can be more aggressive and require a more extensive procedure. But in my experience, these are the exception and only seem to happen in very elderly patients,” adds Dr. Minars.
If a more extensive procedure is required, it may include:
- Surgical excision — this may be standard excision or Mohs surgery
- Radiation
- Injection of chemotherapy drugs directly into the lesion
- Burning and scraping the lesion
Alongside surgery, the following oral medications may also be prescribed:
- Acitretin
- Methotrexate
- Cyclophosphamide
Can keratoacanthoma be prevented?
The same skin cancer prevention advice is true for preventing keratoacanthoma — be sun smart and protect your skin at all times!
- When outdoors, apply an SPF 30+ broad-spectrum sunscreen, even on cloudy days.
- Wear a hat and long sleeves if you intend to be in the sun for prolonged periods.
- Be wary of sitting near windows. For instance, if you drive a car, make sure you protect the arm exposed to the sun. If you sit in an office near a window, remember, the harsh ultraviolet rays can still cause skin damage.
- Conduct regular skin self-examinations.
And most importantly, if you notice anything unusual, visit a dermatologist for diagnosis.









