- Though rare, men do develop breast cancer
- The cause can be primarily attributed to abnormal hormone levels and gene mutations
- Men with inherited cancer-causing gene mutations should undergo genetic testing
- Treatment for male breast cancer is similar to treatment for female breast cancer
What is male breast cancer?
Most of us associate breast cancer with women, but the reality is that both men and women can develop this disease.
Male breast cancer is quite rare—affecting less than 1% of men—according to the American Cancer Society (ACS), with just one in one thousand men receiving a breast cancer diagnosis. Unfortunately, these men have a higher mortality rate than women, primarily due to delaying diagnosis and treatment—even when they notice a lump in one of their breasts. Men are less aware than women that they can develop this form of cancer.
What are the causes and risk factors?
Male breast cancer is believed to be caused by several factors, primarily abnormal hormone levels and gene mutations.
In both men and women, breast cells normally grow and divide as a result of female hormones, such as estrogen. However, the more cells divide, the greater the likelihood that changes to the DNA during this process will lead to cancer. DNA is the molecule that tells the cells how to function. More specifically, certain genes tell our cells when to grow, divide, and die—if the DNA mutates and causes the genes to malfunction, the cells may begin to divide uncontrollably.
Most DNA mutations pertaining to breast cancer in males are acquired mutations; that is, they occur during one’s lifetime as opposed to being inherited. Researchers have yet to determine what causes these mutations, although radiation and carcinogenic chemicals in a person’s diet or environment may be factors.
Other DNA mutations that increase the risk of developing breast cancer are inherited. Inherited mutations of the BRCA1 or BRCA2 tumor-suppressor genes are one of the biggest risk factors for developing breast cancer. As such, men with BRCA1 or BRCA2 gene mutations have a higher risk for breast cancer (as well as other cancers such as prostate or pancreatic cancer).
There are a number of other risk factors. According to Anita T. Johnson, MD, Breast Surgical Oncology Director at Cancer Treatment Centers of America (CTCA) in Atlanta, Georgia, in addition to inherited gene mutations, these include advanced age, liver disease, obesity, radiation exposure to the chest; a genetic predisposition to Klinefelter’s syndrome, and especially exposure to estrogens for the treatment of prostate cancer.
Priyanka Raval, MD, breast cancer medical oncologist at Georgia Cancer Center in Augusta, Georgia, says that testicular conditions, too, can be associated with an increased risk of breast cancer in men. These conditions include orchitis, undescended testes (cryptorchidism), and testicular injury.
“Any other condition that can reduce the testosterone/estrogen ratio can increase risk for male breast cancer,” she adds. “Prior history of chest wall irradiation can also increase the risk.”
The American Cancer Society also cites heavy drinking and estrogen treatment for sex reassignment as risk factors for male breast cancer.
What are the signs and symptoms?
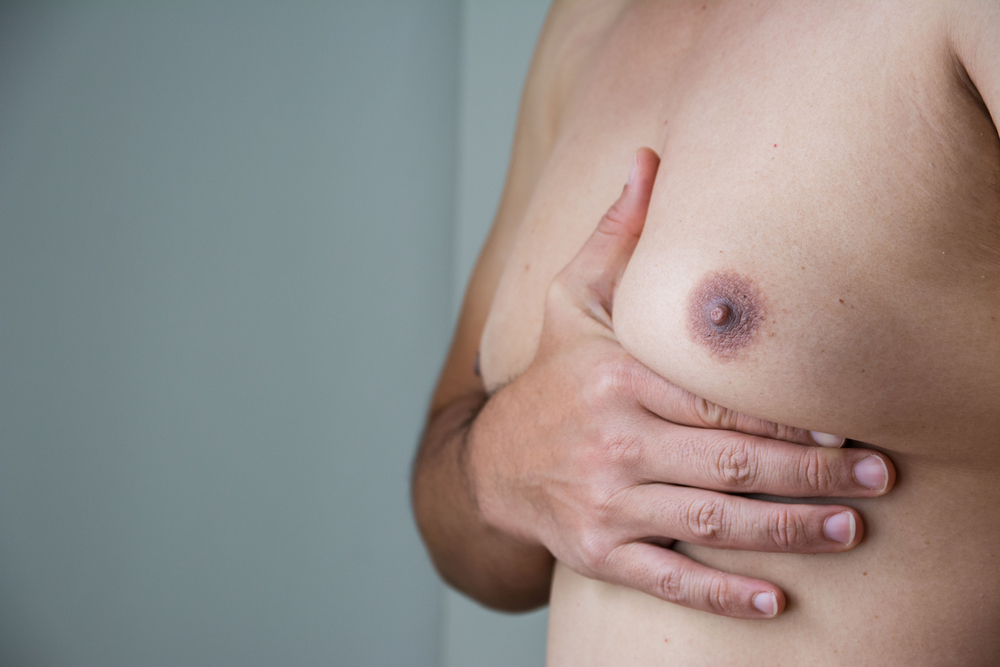
Male breast cancer is typically identified as a hard lump or mass situated under the nipple-areolar complex (the structure comprised of the nipple and the dark skin surrounding it) but may manifest in other ways.
“The mass can feel like a ball, a lump, a thickening, a swelling, or even just manifest as a change in the skin or evidence of an architectural change (or pulling) of the breast,” says Debra Patt, MD, Medical Oncologist at Texas Oncology, and Chair of The US Oncology Network Pathways Task Force for Breast Cancer.
Raval says this mass most commonly presents below the areola, with about half of men having some nipple involvement. In addition, she says, “there can be skin involvement and [the cancer] can present as nipple retraction, ulceration or a mass that is fixed to overlying skin.”
According to Johnson, other symptoms and signs include bloody or clear nipple discharge, inversion of the nipple, scaly changes around the nipple, skin dimpling and enlarged axillary (armpit) lymph nodes.
“Unfortunately, more than 50% will present with enlarged axillary lymph nodes,” she says. “As well, more than 40% present with Stage 3 or Stage 4 disease.”
Raval points out that a breast cancer mass can be confused with other common conditions such as a lipoma, which is usually a softer benign mass comprised of fat cells. “The way to definitively differentiate between these would be with a tissue needle biopsy,” she says.
How common is male breast cancer?
Male breast cancer is uncommon. Johnson says that, in addition to accounting for just 1% of all breast cancers, male breast cancer accounts for approximately 1% of all male cancers. Most men develop the disease between the ages of 60 and 70.
Male breast cancer estimates from the American Cancer Society (ACS) are as follows for 2018:
- 2,550 new diagnoses of invasive breast cancer are expected to occur
- Approximately 480 men will die as a result of breast cancer
What are the treatment options?
There are several treatment options for breast cancer, depending on the patient’s individual needs. Potential treatments include: local treatments, surgery, radiation therapy, systemic treatments, chemotherapy, hormone therapy, targeted therapy, bone-directed therapy, neoadjuvant therapy (medication prior to surgery), and adjuvant therapy (treatment to prevent cancer from returning).
The type(s) of treatment employed will depend on the type of cancer and what stage it is at. Many men may have more than one type of treatment because if one of the aforementioned treatments is unsuccessful, the medical team may recommend trying other options.
Most of the knowledge that experts have of male breast cancer derive from their experience treating female breast cancer. The fact that few men develop breast cancer makes it difficult for researchers to study male breast cancer patients separately. As a result, treatment options for men and women are similar.
But there are also differences in the treatment and surgical approach.
“Surgically, men will require a mastectomy, as breast conservation usually is not desired and is not a recommended treatment option,” says Patt. “Chemotherapy choices and endocrine choices [hormone therapy] are similar, but endocrine choices are a little more complex with men.”
Johnson says that in some cases radiation is needed, and adds that the lymph nodes will be evaluated with either a sentinel lymph node biopsy and or axillary lymph node dissection. She also points out that breast conservation has been reported in the literature with equal survival rates when radiation is added. “Reconstruction can be performed as well with either an implant or autologous tissue,” she says.
Raval echoes Johnson’s thoughts about breast conservation. She says that for men with locally advanced breast cancer, neoadjuvant chemotherapy (medication administered prior to surgery) rather than primary surgery is recommended. And, she says, the approach to men with metastatic (spreading) or advanced breast cancer is similar to that for women with metastatic breast cancer, usually involving chemotherapy or targeted agents.
What is the survival rate?
Statistics pertaining to the prognosis of patients with a specific cancer type are often expressed in the form of five-year survival rates. However, many people live much longer than five years after diagnosis.
A more precise measure is the “relative survival rate,” which looks at men with breast cancer in comparison to the population as a whole. According to the Susan G. Komen organization, a breast cancer organization devoted to addressing breast cancer on multiple levels—including research, community health, global outreach and public policy—the five-year male breast cancer survival rate is 83%. In other words, following breast cancer diagnosis, men with breast cancer are 83% as likely as men without breast cancer to live five years. The 10-year relative survival rate is 71%.
Men with breast cancer have a higher mortality than women with breast cancer. As Patt puts it, “Male breast cancer often presents more locally advanced than female breast cancer as men don’t routinely examine their breasts.” It is very important to note that identifying breast cancer early expands the treatment options and reduces a patient’s risk of death.
If I have male breast cancer, will my children have it?
There is no way to know for certain. However, a family history of breast cancer in a male first-degree relative is associated with an increased risk of breast cancer among men, according to Raval.
“Approximately 15–20% of men with breast cancer have a family history of the disease compared with only 7% of the general male population,” she explains.
All of the experts we spoke with agreed that men diagnosed with breast cancer should be referred for genetic testing.
“If there is documentation of genetic mutation, his siblings, children and parents should be offered testing if deemed appropriate,” says Johnson. “There is a 50% chance that the gene will be passed on to his children.”
And according to Ellen T. Matloff, MS, a certified genetic counselor and the President and CEO of MyGeneCounsel.com, a greater proportion of male breast cancer is hereditary as compared to female breast cancer. “For that reason, every single male with breast cancer is a candidate for genetic counseling and testing, and these services are recommended through a certified provider,” she says.
Importantly, while the risk of developing breast cancer is only 6% higher among male children of a man carrying a mutated gene associated with breast cancer, the risk is 40–80% higher among female children of the same man.
In summary, breast cancer is rare among men. Abnormal hormone levels and gene mutations are primarily responsible for breast cancer in men. If your father has a cancer-causing gene, you are advised to undergo genetic testing. For more detailed information on male breast cancer, visit the website of the American Cancer Society.