- Scabies is a very common skin condition caused by an infestation of mites.
- The most common symptom is a very itchy rash, which may increase in severity if left untreated.
- Prescription topical creams and oral medication are effective at curing scabies.
- Home remedies may help with the symptoms, but won’t cure the actual infestation.
What is scabies?
Scabies is a widespread dermatological condition that currently affects as many as 300 million people worldwide. It is caused by the Sarcoptes scabiei var hominis, a microscopic mite—also called the itch mite— that burrows into the epidermis (the outer layer of skin), where it lays eggs. This typically results in a very itchy rash.
“Scabies infestation is passed from person to person,” explains New York City-based dermatologist Dr. Gary Goldenberg. “It’s highly contagious and can cause epidemics, especially in places like schools, offices, and dorms. One to ten mites can cause an infestation.”
It is important to note that while a scabies infestation may start as a dermatological issue, it can potentially affect much more than the appearance of skin. People with scabies become vulnerable to bacterial infections, and these can potentially lead to a slew of significant health problems, including heart and kidney disease.
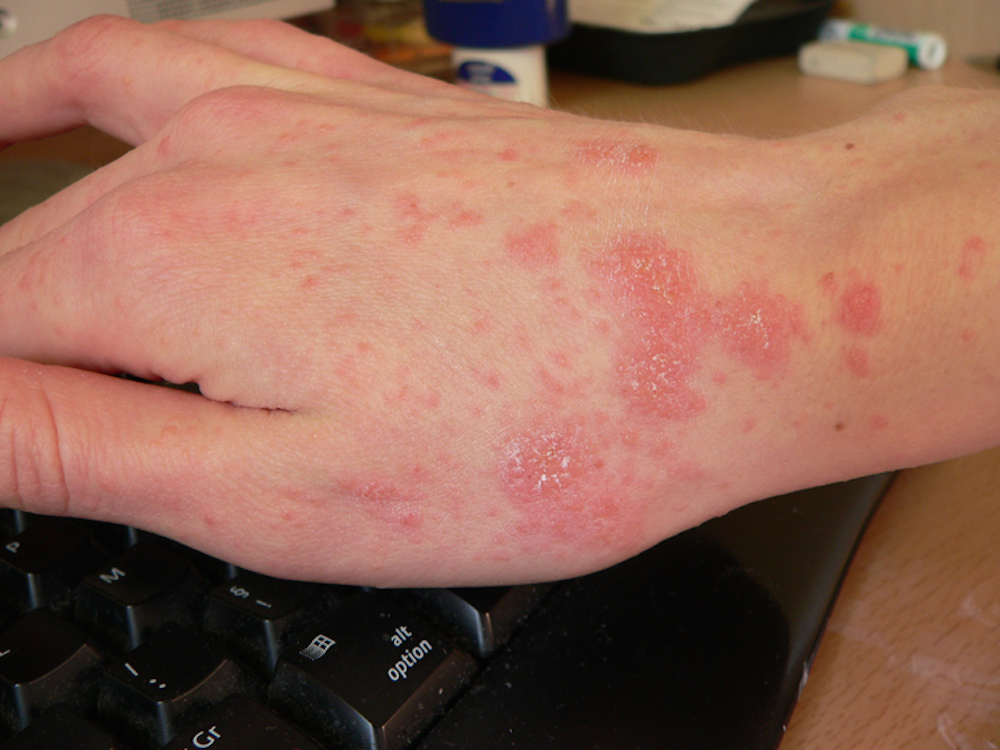
What are the symptoms of scabies?
Given that scabies mites are usually invisible to the naked eye (though large mites may sometimes appear as small white dots), the best way to identify them at home is symptomatically.
If it is your first case of scabies, it may take two to six weeks for symptoms to manifest. If you have had scabies in the past, your immune system will identify the threat quickly and you may notice symptoms within a few days.
Scabies symptoms can vary from person to person, but typically involve:
- Rash – May resemble tiny blisters or pimples on the surface of skin. Grey tracks measuring up to 1.5 centimeters in length may be noticeable; mites create these as they burrow into the skin.
- Intense itchiness – The most common symptom of scabies, the itching is typically worse at night and may be so severe it disrupts sleep. Itching may continue for weeks, even after successful treatment.
- Crusted scabies – If your immune system is compromised, scabies can develop into Norwegian scabies (otherwise known as crusted scabies). Thousands of scabies mites infest the skin, resulting in a scaly rash and other health issues.
Scabies can be quite tricky to self-diagnose as it appears very similar to the rashes caused by many other conditions such as syphilis, dermatitis, and poison ivy. In fact, studies show that traditional tests to diagnose scabies are less than 50% accurate.
As such, it is vital that you see a doctor or dermatologist if you suspect scabies. And if a member of your family or your sexual partner has scabies, it is also recommended that you see a doctor—even if you are symptom-free.
Who is at risk of getting scabies?
While anyone can contract scabies, there are segments of the population that are more vulnerable.
Geography plays a critical role. Scabies is especially prevalent in countries with tropical climates and densely populated regions that enable scabies to proliferate easily. This high rate is also prevalent in communities with high rates of poverty.
Scabies is highly contagious—it is easily spread through skin-to-skin contact, and the sharing of personal items. Children, families (especially those living in crowded conditions), and the elderly residing in nursing homes and residences are therefore particularly susceptible.
Others also at greater risk of contracting scabies include:
- Anyone in close contact with someone infected with scabies
- People with two or more sexual partners
- People of all ages living in long-term care facilities such as dormitories, or military barracks
- People with health conditions that compromise their immune system
What is the best treatment for scabies?
If you think you may have scabies, you need to see a healthcare professional. A doctor or dermatologist will be able to diagnose your skin condition and provide you with an effective treatment plan to resolve the infestation.
Treatment usually takes the form of a topical cream or oral medication. This may be supplemented with prescription and over-the-counter antihistamines, in addition to steroidal creams to manage the itching, pain, and other symptoms.
“Doctors usually diagnose scabies based on symptoms, the appearance of the skin, and sometimes microscopic observation of skin scrapings which reveals the mites,” says board-certified infectious disease physician Dr. Amesh Adalja. “Treatment is usually with a scabicide cream or lotion (e.g., permethrin) applied to the skin or with an oral antiparasitic treatment (e.g., ivermectin).”
Permethrin
To effectively treat scabies, permethrin—a topical cream—is applied to the entire body from the neck down, including under the fingernails, and left on the skin for about eight hours before washing off. This cream can be applied before bed and washed off in the morning.
A single treatment may be sufficient to treat noncrusted scabies. However, it will need to be repeated if live mites are still present after two weeks. For crusted scabies, permethrin is typically used daily for a week, then twice weekly until completely cured.
Ivermectin
In some situations ivermectin may be recommended—a non-FDA approved antiparasitic tablet that is thought to be effective in treating scabies. It is usually prescribed for patients with compromised immune systems, more severe cases of scabies (crusted scabies), and for those who did not respond well to permethrin.
Ivermectin works directly on the mite itself, leading to mite paralysis and death. If taking warfarin (Coumadin), be cautious as it may increase the risk of bleeding.
A single dose of ivermectin with food is usually enough to treat most cases of scabies. In cases of crusted scabies, the treatment is given over a course of several days with a specific dosing schedule.
It is important to consult with your OB/GYN if pregnant or breastfeeding, as ivermectin may not be a suitable option.
Treating scabies with ivermectin commonly causes the following side effects: itch, rash, swollen lymph nodes or fever. Although rare, serious side effects may include low blood pressure, racing heart, asthma exacerbation, allergic reaction, vision issues, and hepatitis.
How to remain scabies-free after treatment
Sanitization is critical to avoid reinfection. In the days and weeks following treatment, it is vital to clean your home meticulously in order to remove mites and minimize the risk of getting scabies again.
We suggest the following:
- Thoroughly vacuum all carpeted floors and upholstery; carefully dispose of the bag after use.
- Thoroughly clean every room in the house with your usual household cleaning products.
- Wash all items of clothing and linen using detergent and hot water.
- Dry all washed items using the hottest temperature cycle.
- Any items that cannot be washed should be placed in a sealed plastic bag for at least one week to ensure all mites are dead.
- Avoid any close contact with anyone who has scabies.
How effective are natural scabies treatments?
The internet is awash with all sorts of DIY solutions for treating scabies—tea tree oil, aloe vera, clove oil, neem oil and cayenne pepper are just some of the natural remedies deemed effective in treating scabies and preventing reinfestation. However, there is no scientific evidence to back up these claims.
As Baltimore family physician Dr. Susan Besser explains, these home treatments are generally safe and may help with the symptoms, but they cannot get rid of the mites that are responsible for scabies.
“Home remedies will help the symptoms (the itching) but don’t actually treat the infestation,” says Dr. Besser. “To treat scabies, you need a prescription for permethrin.”
Professional advice for scabies
Scabies is a very common skin condition that can disrupt your day-to-day life and may potentially lead to more serious health issues. The good news is that permethrin treatment is safe, quick, and effective.
Keep in mind that while ivermectin is also effective, it is not FDA-approved for treatment of scabies, and it can cause side effects—some serious. Talk to your doctor or dermatologist today to find the right advice for your circumstances and to restore the health of your skin.









