Rhinoplasty can help give facial features a more harmonious balance and enhance an individual’s natural beauty. It can also be performed to reconstruct and restore nasal functions.
Here’s what you need to know about this common procedure before scheduling your first consultation with a plastic surgeon.
A brief history of the nose job
Rhinoplasty has been around for at least 5,000 years, with the earliest treatment for the repair of a broken nose first mentioned in the Edwin Smith Papyrus, the oldest known medical work in the world, dating back to ancient Egypt from 3,000 to 2,500 BC.
The procedure was also recorded in ancient India, the Roman and Byzantine Empires, throughout the Middle Ages, and into modern times.
A diverse range of surgeons brought significant contributions to the development of rhinoplasty techniques at the turn of the twentieth century. Dr. Jacques Joseph, an orthopedic surgeon by training, was an early pioneer of rhinoplasty, and went on to become one of the most prolific facial surgeons of all time. In fact, many of the techniques he developed are still in use today.
Rhinoplasty has steadily increased in popularity since the 1950s, and with the development and evolution of the procedure, it has become both more accessible and common. In fact, recent statistics compiled by the American Society of Plastic Surgeons show that over 210,000 people underwent a nose job in 2015.
The aesethetic and functional benefits of rhinoplasty
The procedure’s popularity is in great part due to its versatility.
Rhinoplasty can either reduce or increase the overall size of your nose, straighten a crooked nose, alter the shape of the tip or bridge, narrow the span of the nostrils, or even change the angle between your nose and upper lip. Rhinoplasty can also help patients who require nasal reconstruction to improve their breathing.
Some of the most common reasons to undergo a rhinoplasty procedure include:
- Aesthetic preferences
- Correction of a crooked or prominent nose
- Widening of a thin nose
- Correction of a pointy, upturned or drooping tip
- Correction of flared nostrils
- Smoothing of a bump on the bridge of the nose
- Correction of an asymmetrical nose
- Correction of damage to the nose caused by an accident
- Correction of respiratory issues, such as a deviated septum
- Correction of sinus issues such as sinusitis
How aging affects the nose’s shape
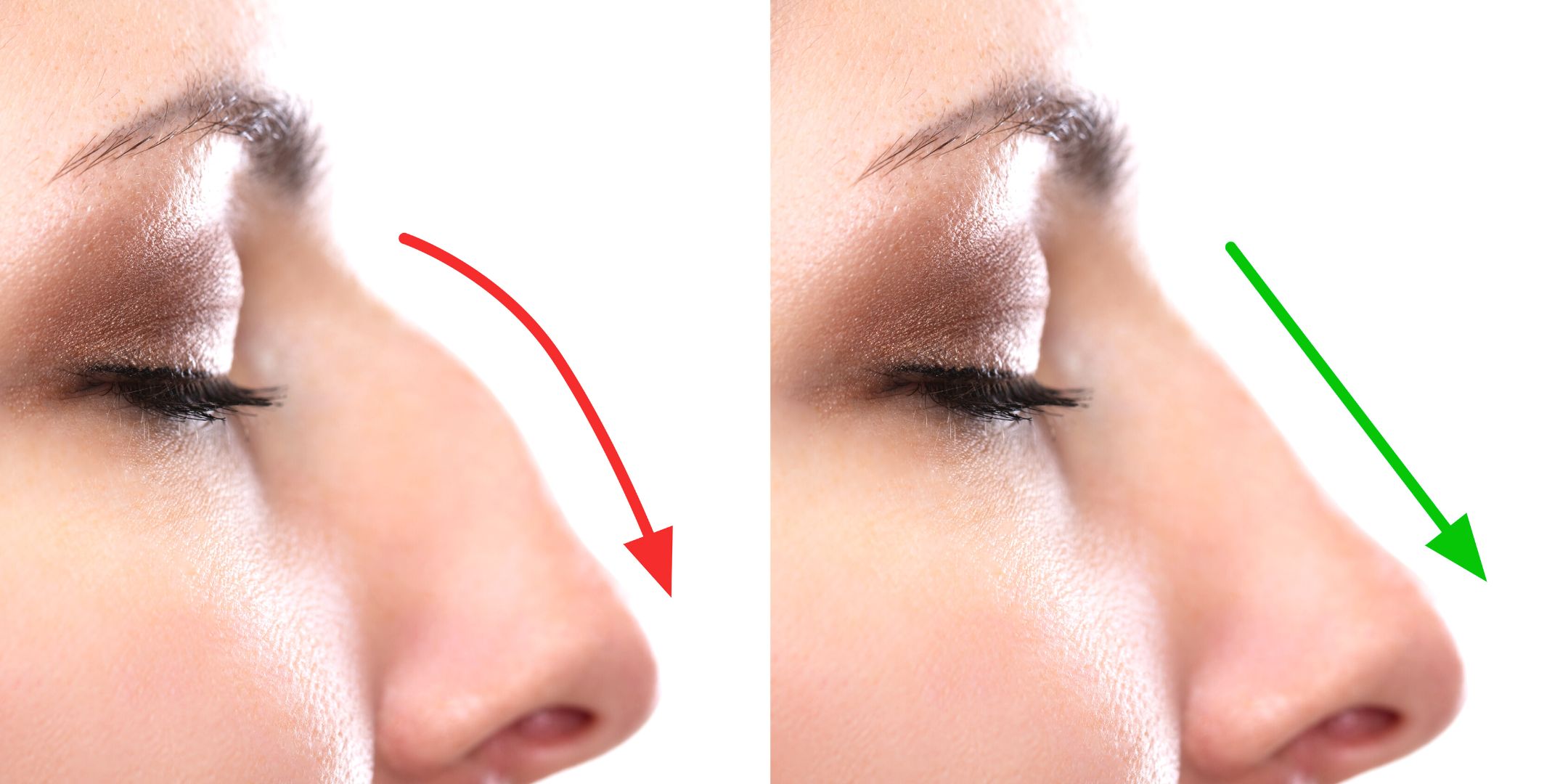
As we age, our noses tend to undergo some predictable changes. The skin thickens as the tip and starts to droop due to gravity. This can give some people the appearance of a bump on their nose. In most cases, however, this isn’t an actual bump, but rather just the appearance of one as the tip slowly moves away from the top of the nose.
This starts to occur as the attachments and support structures within the nose, as well as the skin elasticity outside, begin to weaken. It can happen by the time people reach age their 50s or 60s. In addition, the bone under the tip of the nose and the teeth can start to lose volume, encouraging the tip of the nose to droop further.
Add to that the usual appearance of lines and wrinkles in the skin as we age, and the overall look of the nose simply deteriorates over time.
A remarkably simple rhinoplasty can correct the symptoms of an aging nose. This simplified surgery is only performed on the tip of the nose, utilizing cartilage grafts. No nasal bones are broken, and most patients recover in only about 5 days.
There is no upper age limit for the procedure. That said, to avoid certain risks, you’ll need to be in good overall health. Also, for the best results, you should have good skin elasticity in your face, particularly around the nose.
What to expect during your initial consultation
Even though the actual rhinoplasty surgery might be relatively short, usually lasting only a few hours, the entire process, from booking your initial consultation through to the end of your recovery, requires a much larger time commitment.
The very first thing you’ll do during your preparation for a nose job, well before any surgery is scheduled, is meet with your surgeon to discuss a variety of important factors. This will determine if you’re a good candidate for the procedure to begin with.
Your consultation will likely involve a frank discussion about your motivations for the surgery and what you expect from it.
Your surgeon will need to know if you have any chronic medical issues, as certain conditions could make you an unsuitable candidate for surgery. As such, you will also be asked about your medical history, including any nasal obstructions or prior surgeries you’ve undergone, as well medications you’re currently taking.
This initial meeting will most likely involve a complete physical exam, including a series of lab tests. The skin lining both the inside and outside of your nose will be inspected. This exam helps to give your surgeon a better idea of what needs to be changed, and how your unique facial features might affect the results.
Sometimes this physical exam also includes taking photographs of your nose from different angles. Your surgeon might use a computer application to manipulate these photos to show you what results are possible with your specific features.
These photos provide no guarantee of how you’ll look after surgery; instead, they simply offer a prediction of the kind of results you might expect.
Maintaining realistic expectations
Before you decide to undergo rhinoplasty, it’s important to understand the procedure’s limitations so you can enter in to it with realistic expectations. Rhinoplasty has a higher dissatisfaction rate than most other cosmetic procedures, usually because of three reasons:
- The surgeon misunderstands the patient’s aesthetic goals.
- The patient has impossible expectations.
- The failure to achieve these expectations.
While many surgeons encourage patients to present them with images of noses they both do and don’t like as a starting point, it’s essential to understand that rhinoplasty can’t make you look like someone else or offer you a completely different nose.
Each person has their own, unique facial structure that plays an important role in determining which nose shape and size will work best for them.
When considering rhinoplasty it’s a good idea to make sure you fully understand what the procedure is and isn’t capable of. Rhinoplasty requires such a high level of surgical precision that even a 1 millimeter change can dramatically impact results.
Your goal should be to subtly adjust your nose to better suit your face, not to wake up looking like a different person.
Rhinoplasty costs: budgeting for your nose job
When calculating the overall cost of your rhinoplasty procedure, there are three basic fees to keep in mind:
- Anesthesia fees
- Your surgeon’s fees
- Hospital or surgical facility fees
On average, your surgeon’s fee for rhinoplasty will make up the majority of the total price. However, it doesn’t include either the anesthesia fee or the surgical facility fee.
Anesthesia costs usually range from $600 to $1,200, and facility fees are often between $700 and $1,100. This can bring the total investment for rhinoplasty to between $5,000 and $10,000.
Other factors that affect the overall cost include the extent of your surgery, its complexity, and your surgeon’s reputation. The geographical location where your surgery is performed also has a bearing on its cost, since clinics in busy cosmopolitan centers often charge more because of higher overheads.
If cost is an issue that is inhibiting you from undergoing rhinoplasty, most surgeons offer flexible, monthly financing plans. Third-party financing options are also available. These often take the form of “medical credit cards,” which work exactly like a normal credit card, except they are specifically designed for elective surgeries.
Preparing for rhinoplasty surgery
The following tips will help ensure that your procedure goes as smoothly as possible.
- Avoid blood thinners.
About two weeks before rhinoplasty you should stop using any aspirin, Ibuprofen, Vitamin E, or other herbal supplements you might be taking. These medications can interfere with your body’s natural ability to form blood clots and generally heal.
- Don’t smoke.
If you’re a smoker, you’ll need to stop smoking at least two weeks before your rhinoplasty. Nicotine in the bloodstream can negatively affect healing, prolonging bruising and swelling. Quitting is the best way to ensure your nose heals well and without unnecessary complications.
- Run your errands beforehand.
Consider stocking up on household supplies and fill your prescriptions ahead of time so you don’t have to go out in public. Compared to many cosmetic procedures, the recovery period for rhinoplasty is relatively short. That being said, many people feel self-conscious about the facial bandaging that is necessary immediately after the procedure.
- Ask for help.
See if you can enlist the help of a relative or friend for the first few days and nights post-op. You might still feel a little groggy after the surgery so it’s nice to have someone around to help you out and keep track of when you’ve taken your medication.
- Stock up on lip balm and beverages.
Following your surgery, you’ll be breathing through your mouth for a little while. Because of this your mouth will get very dry and possibly a little uncomfortable. A humidifier is also a good idea.
- Arrange transportation beforehand.
You will not be able to drive yourself home after the procedure. In fact, you’ll most likely need a trusted friend or family member to be with you in order to be discharged from the surgical facility.
Rhinoplasty techniques
Rhinoplasty has the ability to adapt to the goals and needs of each patient, so the procedures themselves can vary widely based on individual needs. However, they all generally start with the same step: anesthesia. There are two sedation methods available for rhinoplasty: general and IV sedation.
General anesthesia is administered with a mask or IV, and will put you completely to sleep. IV sedation, on the other hand, is different. Your doctor will first numb your face with a local anesthesia and then give you a powerful sedative through an IV line. You’ll experience a “twilight sleep,” and probably not remember much, if anything, of the procedure afterwards.
The method that is more suitable for you will be something you’ll discuss with your surgeon ahead of time. Once you’re fully sedated, the procedure can begin.
There are two primary approaches to the rhinoplasty procedure: “closed” and “open.”
Closed or endonasal rhinoplasty
The endonasal rhinoplasty approach gets its name from the fact that all the surgical reshaping is carried out inside the nose, without any visible incisions made to the face. Incisions are made along the inside of each nostril, called “marginal incisions,” and are performed in an arc shape that follows the curve of the alar cartilage.
Next, through the nostril, another incision is made between the alar cartilage and the upper lateral cartilages (ULC), called the “intercartilaginous incision.” Through these incisions both the tip and the bridge of the nose can be reshaped with no external scarring.
In the case of tip reshaping, or structural rhinoplasty, your surgeon will make both the marginal incisions and the intercartilaginous incision together. Once completed, the alar cartilage can be pulled out of the nostril and reshaped. A great deal of nasal tip shaping can be achieved with the closed approach, especially if your surgeon has experience with this technique.
In the case of bridge reshaping, the intercartilaginous incision is the most important as it allows access to the middle and upper parts of the nasal bridge. Through this incision, the skin of the nose is lifted off the underlying cartilage and bone to allow for reshaping.
Once this is completed, a retractor is put in place to keep the skin elevated while your surgeon addresses the bone and cartilage. This can all be performed through your nostrils. The closed approach has had significant success in reducing the nasal bridge height, and is used in osteotomies, where the nasal bones are carefully and skillfully broken to narrow or straighten the bridge.
The closed technique can have very successful results, but most surgeons agree this method is more difficult because they can’t see what they are doing as well. The surgeon is essentially operating “blind.” Imagine trying to fix some broken pottery under a sheet. It’s not impossible, but certainly difficult. Choose an experienced surgeon in this technique for the best results.
Open or external rhinoplasty
The “open,” or external, approach to rhinoplasty accesses the nose via a small, inverted-V shaped incision across the columella, connecting the nostrils. With the addition of some internal incisions, the entire nasal skin can be folded back, almost like the hood of a car.
This gives your surgeon a much better view of the internal structures of your nose. With this extended view, your surgeon can assess nearly the entire nasal framework. This allows them to be as symmetrical as possible in the procedure, since the entire nose can be visualized at once, rather than through separate incisions as in the closed technique.
Once the nasal cartilages have been exposed, your surgeon can reconstruct the whole area by reducing, reshaping, and suturing. Cartilage grafts from other parts of your body can also be used to maintain the shape and form of your nose. Results tend to be more predictable with this approach. A significant downside, however, is prolonged swelling of the nose.
Septoplasty
Septoplasty is a particular surgical procedure designed to correct a deviated septum. The septum is the bone and cartilage structure that separates your nostrils and runs down the center of your nose. When it displaces to one side or the other it can narrow one nostril and cause breathing issues.
During a septoplasty, your septum is straightened and repositioned in the center of the nose. This should correct any airway problems and will often address chronic snoring.
This is achieved by lifting the lining of both sides of the septum through small incisions inside the nose. Through these small incisions, your surgeon can remove part of the septum, and realign it so it is straight.
Once the septum has been fixed, nasal splints can be placed inside the nose to help with healing, and the lining of each side of the septum is replaced. Stitching may be used to help the lining heal properly.

RELATED: What to Expect During and After Septoplasty
Rhinoplasty recovery
Usually, the recovery time from a nose job is about two weeks, but because each surgery is tailored to meet your facial structure and goals, the actual recovery time will vary from patient to patient.
The length of your recovery will depend on a number of factors, including:
- The extent of the surgical changes to be made
- How closely you follow post-op guidelines
- Your overall health before surgery
The first 24 hours
For a lot of patients, the first 24-48 hours of recovery are the most difficult.
You’ll still likely be feeling some of the effects of the anesthesia and might experience some mild discomfort. Your nose will ache, you might experience a dull headache, and your face will probably feel puffy. Some bleeding is also normal.
Swelling is an expected side effect immediately following rhinoplasty. To help reduce this swelling and keep your recovery moving forward, it’s best to spend the first 24 hours comfortably in bed with your head elevated. Sleeping promotes healing, so if you have the opportunity to nap, take it.
Your surgeon can give you a prescription for pain medication if it gets too bad, but most people only need over-the-counter medications. Either way, stay on top of your medication schedule. Pain after a rhinoplasty is usually fairly mild but it can exacerbate quickly. If you’re not staying on schedule with your meds it can be difficult to get it back under control.
Remember not to blow your nose for a while, because this forceful action too early in your recovery can have a detrimental impact on your results. Also avoid airline travel right after surgery, as the changes in pressure can affect results.
After a week
About a week after your surgery you’ll likely have a follow-up appointment so your surgeon can keep track of your progress. If your procedure involved nasal packing it will be removed at this time, along with any splints and stitches. Your bruising should start to fade, and swelling will begin to subside.
Most patients are able to go back to work and get back into a normal routine about a week after their nose job. Even if you are able to resume most of your normal activities, it’ll still important that you stay cautious and avoid strenuous exercise for at least two weeks.
It’s also important to avoid bumping your nose as it heals. That means watching out for pets, small children, and anyone you share a bed with.
Note that you may still experience some discomfort and soreness radiating from your nose into your mouth and jaw. Stick to soft foods for the first week or two to help ease this pain.
The following months
For most patients, the satisfaction they feel after their rhinoplasty far outweighs any pain or discomfort they might experience during recovery. Nearly all the side effects of this procedure fade relatively quickly.
That said, it’s important to keep in mind that some minor swelling might persist for several months. In the end, it might take up to a year for the final, full results to be revealed.
As a last word of advice, keep your nose out of direct sunlight for a few months after surgery. Sunscreen and hats help promote healing and reduce swelling.

RELATED: Rhinoplasty Recovery Advice You Need to Follow
Post-recovery results
Rhinoplasty often makes very small changes to the structure of your nose, sometimes changes as small as millimeters. But these small changes can make a huge difference in how your nose looks.
That said, the results of rhinoplasty are often more difficult to predict than with other cosmetic procedures, and rhinoplasty results tend to have a higher dissatisfaction rate.
In up to twenty percent of cases, additional modification of the nose is necessary to either achieve, or maintain, your desired results. Be sure to stay in contact with your surgeon during and after your recovery to ensure you are fully satisfied with your new nose.
Scarring
Just like all surgeries, there’s always the possibility of scarring following rhinoplasty. In the case of a closed procedure, all the scarring will be inside the nose, effectively invisible.
In the case of open rhinoplasty, usually the only external incision is very small, across the columella between the nostrils. Because this incision is so small and on the underside of your nose, even if it doesn’t completely fade it’s generally not noticeable.
Risks and potential side effects
When performed by a qualified and experienced cosmetic surgeon, a rhinoplasty is a very safe procedure with few, if any, long-term complications.
Temporary side effects of rhinoplasty usually fade within a few weeks, and include:
- Bruising around the eyes
- Soreness and swelling
- Swelling
- Inflammation of the sinus passages
- Nosebleeds, generally within the first 72 hours
Some rare, but more serious rhinoplasty complications may include:
- Infection
- Negative reaction to anesthesia
- Unsatisfactory results, including asymmetry
- Noticeable scarring
- Numbness
- Serious breathing difficulties
- Chronic nosebleeds
- Perforated septum
- Burst blood vessels
- Hematoma, which is a collection of blood beneath the skin
- Possible revision surgery
Latest rhinoplasty techniques and scientific studies
Rhinoplasty is one of the most technically demanding facial cosmetic procedures. As a result, surgeons consistently seek to revise their surgical techniques to ensure the highest possible understanding of nasal aesthetics and soft/hard tissue dynamics to achieve a balance of form and function.
Moreover, individual patients’ anatomies mean a customized approach is paramount to ensure any medical factors that may impact on the final outcome are taken into account.
Computer modeling and simulation is a recent development that holds the potential to revolutionize how rhinoplasty is performed. Modeling has been successfully used for decades in fields such as engineering, helping engineers conceptualize and design complex processes. With the development and advance of computing technology, applications for modeling and simulation have gradually expanded to the medical sphere.
A 2017 report in the Facial Plastic Surgery Clinics of North America notes that modeling can now be applied to rhinoplasty techniques to help surgeons make more informed decisions about the most effective maneuvers to achieve an optimal aesthetic outcome.
Modeling also takes into account a patient’s specific anatomy while ensuring that any clinical requirements are also considered, thereby promising rhinoplasty closely tailored to the individual.
Another influential development in rhinoplasty is research into the use of silicone-polytetrafluoroethylene (PTFE) implants with a silicone core and PTFE liner. Nasal implants are mainstays of Asian rhinoplasty and also used for individuals with smaller noses who want greater nasal height. However, silicone and Gore-tex implants sometimes provoke a foreign body response and are prone to migration (movement once inserted). A 2017 study trialled these composite implants on 177 patients and revealed promising results.
Watch this space for more details as further information is released.
Frequently asked questions
Are there non-surgical rhinoplasty options?
Recently a nonsurgical alternative to rhinoplasty was developed using dermal fillers to enhance the shape of the nose. Also known as a liquid nose job, this injection treatment is ideal for correcting minor issues like smoothing a bump on the bridge or adding volume to the tip.
It generally takes only a few minutes to complete, with results lasting a few months (at most), depending on the injectable filler product used.
Unfortunately, if you’re looking for major changes, need a reduction, or require treatment to correct a deviated septum, surgery is the only viable option.
Rhinoplasty, mentoplasty… or both?
Rhinoplasty addresses issues in the nose. Mentoplasty, or genioplasty, on the other hand, is a cosmetic procedure designed to augment a receding chin. To increase the chin’s “projection,” or in other words, how far it protrudes, the patient may choose a medical grade synthetic implant, or have their bone structure altered (also known as sliding genioplasty).
While it’s true that most people focus on the nose when thinking about undergoing a cosmetic facial surgery, it’s not the only way to achieve a particularly pleasing profile. More and more patients are either combining their rhinoplasty with a mentoplasty, or simply choosing to undergo a chin augmentation alone.
For the most pleasing profile, your chin should closely line up with your upper lip and be slightly angular. A weak chin can give the impression of asymmetry in the face, or even make the rest of your facial features seem disproportionate. This means that if you have a weak chin it your nose could appear bigger than it really is.
These procedures are often combined, but in many cases both procedures are not necessary. In fact, depending on the shape and composition of your facial features, a chin augmentation can make your nose seem smaller and more proportionate, completely eliminating the need for a rhinoplasty. Be sure to discuss all of your options with your surgeon.
Am I too young to get a nose job?
In general, ideal rhinoplasty candidates are older than 15 (for girls), or 16 (for boys). This is because the American Society of Plastic Surgery (ASPS) recommends waiting until the nose has finished developing before undergoing rhinoplasty. This can be different for everyone, but these ages offer a good guideline.
What is ethnic rhinoplasty?
When performing rhinoplasty, the surgeon’s goal is to give the patient a nose that best suits his or her unique face. Ethnic rhinoplasty does this while ensuring that the patient’s ethnic characteristics are preserved.
Most ethnicities have fairly distinct facial characteristics, and in many cases, the nose is one such feature. An “ethnic” rhinoplasty is simply a normal rhinoplasty procedure that aims to give the patient the desired aesthetic changes while making sure the nose stays true to their facial characteristics and ethnic background.
This is particularly important when considering the extent to which the bridge, nostrils and tip can be changed.
Can I wear glasses during rhinoplasty recovery?
Don’t wear glasses as you normally would for at least four weeks after your rhinoplasty. Resting glasses on your nose can seriously disrupt its healing, especially if you’ve had bones broken during the surgery.
If you must wear glasses, try either taping them to your forehead, or use some sort of foam or pad as a cushion between your glasses and nose. A splint or “frame up” to prop them up off your nose can also help.
Is revision (secondary) rhinoplasty common?
Revision, or secondary rhinoplasty, is performed to correct the shape or function of the nose after a failed or flawed primary rhinoplasty, which occurs in about 5%-20% of all procedures.
This procedure is much more complex than a primary rhinoplasty because it has to deal with scar tissue from the previous surgery. It often requires the nose to be rebuilt using grafts from the nasal septum, ear cartilage, or rib cartilage, as well as synthetic implants if necessary.
Glossary of nose and rhinoplasty terms
Ala (plural: alae): Commonly referred to as the nostril. These are crescent-shaped, and surround the nostril openings.
Alar cartilages: Also called the lower lateral cartilages, these are flexible arches of nasal cartilage that determine the shape and strength of the columella, nasal tip, and alar rims.
Bulbous tip: A cosmetic issue characterized by a wide, oversized nasal tip with large alar cartilages.
Cartilage graft: A piece of cartilage taken from another part of the body (ribs, ear, etc.) custom shaped to strengthen or reshape the nasal skeleton.
Columella: The central “column” that is between the nostrils, as seen from below. It’s made of skin, and the paired right and left medial crura.
Dorsal: This refers to the nasal dorsum, or bridge.
Intermediate crus (plural: crura): The part of the alar cartilage that is above the nostril, but below the nasal dome.
Lateral crus (plural: crura): A part of the alar cartilage. This extends above the nostrils.
Medial crus (plural: crura): The bottom-most part of the alar cartilage.
Middle vault: The middle third of the nose. This is made entirely of cartilage, and is formed by the mid-line dorsal septum and the upper lateral cartilages.
Nasal domes: The hinge-point of each alar cartilage. These define the nose’s tip.
Nasal tip: Also called the “lobule,” this is the forward-most part of the nose, and is formed by the alar domes.
Radix: The nasal root, located between the eyes. This is the upper limit of the nasal bridge, and roughly corresponds to the deepest parts of the nasal bone.
Septum: The dividing wall between the right and left nasal passages. This is formed by cartilage and bone and is covered with a layer of nasal mucosa.
Tip projection: This term refers to how far the nasal tip extends from the vertical plane of the face.
Upper lateral cartilages (ULC): The cartilage structures that make up the medial vault.