- Skin ulcers are open sores that fail to heal properly.
- There are many different types of skin ulcers, each requiring an individualized treatment plan.
- An open sore that won’t heal is cause for concern and should be evaluated by a physician.
Although we don’t often think of it as such, skin is technically a body organ—and the largest one at that. It serves many functions including physical protection against the outside environment and heat regulation. It’s also one of the first lines of defense against pathogens like bacteria and viruses.
Chronic skin ulceration significantly impacts those functions, causing inflammatory conditions, infection, and in extreme cases can even lead to amputation and mortality.
Here we examine the classification, diagnosis, and various treatment options for the most common types of skin ulcers.
What are skin ulcers?
An ulcer is a break or erosion of the skin or mucous membranes (such as the inside of the mouth or the lining of the stomach) that contains damaged tissue and inflammation.
Ulcers are slow to heal, and in some cases may fail to heal entirely.
To be technically classified as a skin ulcer, the break must involve the entire thickness of the outermost layer of the skin (epidermis), but it may also extend deeper into the skin.
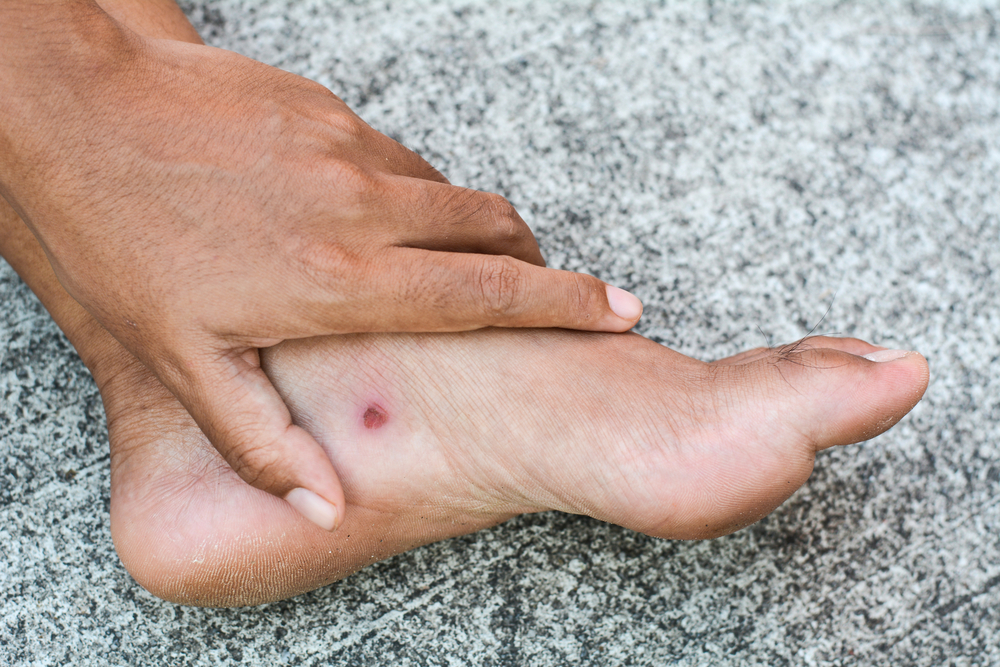
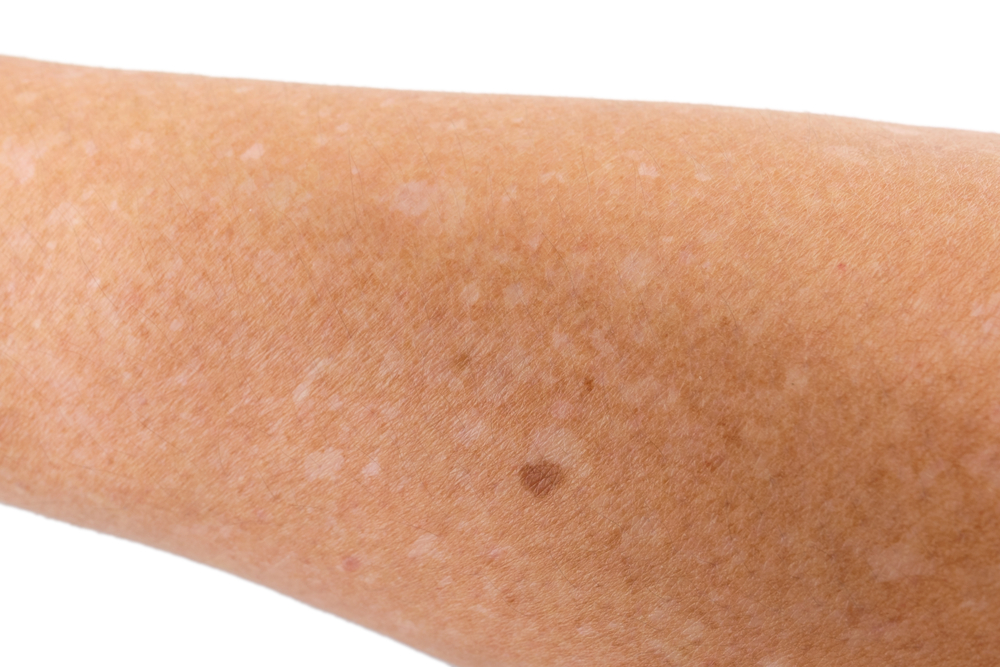
What do skin ulcers look like?
Ulcers look like open craters or sores that may ooze blood. Most ulcers are associated with inflammation, making them red, painful, swollen, and warm to the touch. Necrotic (dead) tissue in the ulcer may appear black.
If the ulcer begins to discharge pus, develops an offensive smell, or if you develop a fever, this could mean that the ulcer has become infected.
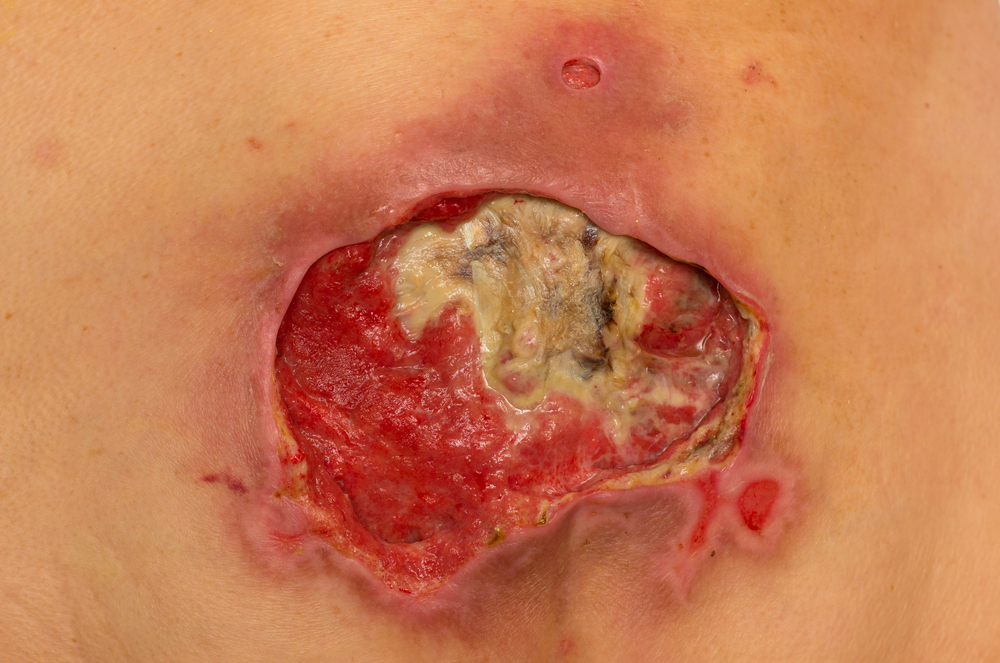
Ulcers due to poor blood circulation
Good blood flow is essential for the maintenance of healthy tissue. If blood flow to an area of the body is interrupted or poor, the tissue may begin to disintegrate, causing healing to be sluggish and ineffective.
Blood is carried through the body within arteries (that carry blood from the heart to the tissues) and veins (from tissues to the heart). Problems with either can result in blood flow interruption and ulceration.
Arterial ulcers
Several diseases can damage arteries, impairing their ability to deliver blood to tissues. This is most commonly due to diabetes and atherosclerosis (hardening of the arteries), which is related to smoking, high cholesterol, heredity, and hypertension.
Arterial ulcers are often cold, dry, and associated with moderate to severe pain.
Venous ulcers
The walls of normal veins have tiny inner structures that resemble one-way flow valves to keep the blood moving forward toward the heart. Venous insufficiency, or damage to the valve system, can cause blood to back up in the veins, building pressure and impairing blood flow.
This commonly occurs in people with varicose veins (dilated and swollen veins). It can also be related to obesity, lack of physical activity, and a history of DVT (deep venous thrombosis; a blood clot that forms in the deep veins of the leg).
Venous ulcers are generally less painful than arterial ones, but they have a greater degree of swelling and more discharge.
Where do they occur?
Arterial and venous ulcers most commonly occur in the lower extremities. Arterial ulcers are generally confined to the feet—usually at the toes or heels—while venous ulcers commonly occur at the ankles.
How are they treated?
Treatment involves wound care and restoration of normal blood flow. Depending on the cause, the approach to flow restoration will differ.
In arterial problems, surgery to widen the lumen of the artery may be required. According to Dr. Kurtis Kim, a Baltimore-based vascular surgeon, there are two ways of achieving this:
- The surgeon can make a tiny hole in the wall of the artery and mechanically widen its diameter from the inside. This is minimally-invasive surgery.
- Another option is open surgery to completely bypass the affected artery.
Venous ulcers can be managed by external compression stockings. This can stop the blood from backing up in the veins and relieve the symptoms. In more advanced cases, it may be necessary to completely get rid of the problematic veins through various techniques to prevent recurrence.
Neuropathic ulcers
Neuropathic ulcers occur due to problems with nerves. Damage to peripheral sensory nerves— particularly in diabetics—can cause the loss of sensation in parts of the feet. Over time, this can lead to repeated small injuries that go undetected and untreated. The damaged tissue is unable to heal, deteriorates, and eventually forms an ulcer.
Blood vessel injury also occurs in diabetics and promotes the development of ulcers. Neuropathic ulcers can be very deep and the bone may even be exposed in some cases. These ulcers are generally painless.
Where do they occur?
Neuropathic ulcers generally occur on the heels and soles of the feet. This area bears the entire weight of the body when standing; when deprived of sensation, feet may be exposed to extra stress without a pain feedback mechanism that tells the individual to rest.
How are they treated?
Aside from regular wound care, minimizing stress and preventing further injury is very important for halting the progression of these ulcers. Diabetics are advised to examine their feet daily to check for new injuries or skin changes and to wear special shoes that minimize stress on the feet.
Successful control of blood sugar levels in diabetics can help the ulcers heal and prevent the appearance of new ones. Ulcers in people with uncontrolled diabetes may become gangrenous (severely infected). In these cases, amputation of part of the limb is often unfortunately necessary—otherwise, the infection may spread and kill them.
Pressure ulcers
Commonly known as bedsores, these ulcers are caused by prolonged immobility and pressure on a body part. This compresses the blood vessels and interrupts the circulation to this area, resulting in tissue death. These types of ulcers are often seen in bedridden and wheelchair-bound patients.
Where do they occur?
Bed sores are often found on the lower back, hips, back of the head, shoulders, elbows, and heels.
How are they treated?
Pressure relief is the most important component of treatment. Bedridden patients, including those in a coma, should be moved every two hours and those in wheelchairs should change their position every 15 minutes.
Special mattresses, pillows, and cushions can be used to relieve the pressure and distribute the patient’s weight more evenly. Careful wound care and dressing will allow the ulcer to heal more quickly.
Malignancy-related ulcers
Skin cancer, particularly basal cell carcinoma (BCC), squamous cell carcinoma (SCC), and melanoma can erode the skin and cause nonhealing ulceration. However, some ulcers can form inside the body due to cancer under the skin—breast or bone cancer growing close to the surface of the skin may produce an ulcer.
Where do they occur?
Skin cancers tend to occur more in sun-exposed areas of the body such as the ears, nose, forehead, upper lips, shoulders, and the back and lower legs. However, some ulcers can develop internally due to cancer under the skin—an ulcer can be a result of breast or bone cancer growing close to the surface of the skin.
How are they treated?
Most skin cancers are diagnosed early before they have had the chance to spread to other organs, and surgical excision of BCC and SCC is often effective. Other treatment options may include radiation, local chemotherapy or cryotherapy (freezing).
If detected early, the outcome is generally good. For cancers that are growing near the surface of the skin causing an ulcer, the appropriate treatment would be determined by their respective oncology-surgical team.
Genital ulcers
These are generally contagious in nature and related to STIs (sexually transmitted infections) such as herpes, chlamydia, syphilis, and chancroid. Practicing unsafe sex and having multiple sexual partners are the main risk factors for acquiring these infections.
Where do they occur?
They can occur on or around male and female genitals and may be painful or painless. Oral sex with an infected individual may also lead to similar infections appearing in the mouth.
How are they treated?
Bacterial infections like chlamydia respond to antibiotics, while viral infections like herpes respond to antivirals. One caveat is while herpes sores may go away, the organism itself may lie dormant in the body and reappear after a while.
When is surgical intervention necessary?
“Deeper ulcers can require serial debridements surgically depending on the precise location of the lesion,” says Chicago facial plastic surgeon Dr. Benjamin Caughlin. Signs of infection also necessitate surgical intervention.
“If the tissue appears dead or obstructive to healing of specific areas then debridement (surgical removal of damaged tissue) can be helpful,” adds Dr. Caughlin.
Do at-home remedies work?
At-home remedies are not recommended. A skin sore that does not heal is cause for concern and should be evaluated by a physician in order to identify the underlying cause and formulate an effective treatment plan.
According to Dr. Caughlin, early treatment is of extreme importance in achieving a successful treatment outcome.
Need professional skin care advice? Use Zwivel’s online consultation tool to contact a board-certified dermatologist in your area