If you find your breasts hinder everyday activities, or you simply desire cleavage that is better proportioned to your body, breast reduction surgery could be an option worth considering. In the hands of a skilled plastic surgeon, more modestly-sized breasts that are also aesthetically beautiful can be achieved.
Updated, September 2017
What Is Breast Reduction Surgery?
Breast reduction surgery, also known as reduction mammoplasty, decreases the size and weight of overly large breasts and re-contours them to better match the patient’s proportions. The procedure has one of the highest patient satisfaction rates of all plastic surgery procedures, with 95.4% of patients stating satisfaction in a recent survey. More than 114,000 women underwent breast reduction in 2014, a massive 183% increase since 1997.
For most women, the appeal of breast reduction stems from a desire for an improved quality of life. Women with disproportionately large breasts regularly experience increased neck and back pain, sleeping problems, skin irritation, chafing and difficulty exercising. However, the emotional burden of overly-developed breasts is very real too: self-confidence and insecurity issues related to breast size often have a detrimental affect on women.
Breast reduction holds the potential to be life-changing for many patients with myriad psychological benefits, enabling women to feel empowered and capable in their bodies again, rather than held back by their breasts.
According to Dr. Kelly Killeen, a board-certified plastic surgeon and expert in breast surgery, the surgery holds a range of benefits. “This procedure makes people feel better. But the wonderful icing on the cake is that they end up with beautiful, perkier, more youthful-looking breasts in better proportion to their body.”
Through the removal of excess glandular tissue, fat, and lax skin, surgeons can not only render the breasts smaller, lighter and more symmetrical, but also lift the breasts, leaving them firmer, less prone to sagging, and more youthful-looking. Nipples and stretched areolas can also be reduced and cosmetically improved during the procedure.
Other benefits of surgery include bras fitting comfortably, a more balanced and attractive overall silhouette, and enhanced self-confidence when wearing swimsuits and form-fitting garments. Freedom of movement and self-expression in clothing choices are also cited among the greatest benefits of reduction mammoplasty.
Am I a Good Candidate for a Breast Reduction?
If any of the following conditions sound familiar, it is likely you are a good candidate for a breast reduction.
- Breasts that are disproportionate to the rest of your body
- Poor posture caused by heavy breast weight
- Grooves in shoulders caused by bra straps struggling to support the weight of the breasts
- Back, neck or shoulder pain caused by heavy breasts
- Breasts that droop significantly, with nipples that point downwards
- Asymmetrical breasts, with one significantly larger than the other
- Difficulty sleeping or lying down due to discomfort caused by breasts
- Rashes or skin infections affecting the skin beneath the breasts
- Self-consciousness arising from breast size
- Inability to exercise because the breasts hinder physical movement
Ideal candidates for reduction mammoplasty are physically healthy, do not smoke, and do not suffer from medical conditions such as diabetes or heart disease, which can increase the likelihood of complications.
If you regularly experience any of the issues mentioned above and have realistic expectations about what the surgery can achieve, it may be timely to consider talking to a plastic surgeon about the possibility of a reduction and the benefits it could bring you.

RELATED: How to Measure Your Bra Size
Finding a Surgeon
Finding the right surgeon for the job is paramount to any cosmetic surgery procedure. The surgeon you ultimately select to carry out your breast reduction is a choice that you will live with for the rest of your life. Successful breast reduction surgery positively impacts on your self-esteem and offers a greater quality of life. On the other hand, breast reduction surgery carried out by an inexperienced surgeon increases the likelihood of unsatisfactory results, heartache and the potential need for additional investment to correct poor results via revision surgery.
Things to check for:
1. Board certification
The most consistent yardstick of a surgeon’s skill is if they have board certification. The American Board of Plastic Surgery (ABPS) is widely considered the most prestigious plastic surgery board in the United States. When you’re first seeking a plastic surgeon, always be sure that they have ABPS certification. This certification guarantees that the surgeon has undergone rigorous training, has specialization in their field, and observes high patient safety standards.
State medical board certification does not represent an adequate measure of surgeon proficiency, as it is no guarantee that the surgeon has had residency training in cosmetic surgery techniques which often require unique aesthetic expertise.
2. Experience in the procedure you are undergoing
While board certification offers an excellent overall guarantee of a surgeon’s proficiency, it does not guarantee specialization in the specific procedure or reduction technique you are undergoing. Procedures such as as breast reduction surgery, breast reconstruction and breast augmentation actually require dramatically different skills and expertise.
When you begin looking for a surgeon, ensure they specialize in breast reduction surgery, or at least have extensive experience performing it. You may wish to ask your surgeon the following questions:
- How long have you been performing breast reduction surgery?
- What is your training background, and how did you achieve specialization in this procedure?
- How many times have you performed breast reduction surgery?
3. Before/after photographs
Asking to see pictures of the work that the surgeon has completed on former patients also represents an effective way to assess their experience and proficiency. Furthermore, checking out photos of work that the surgeon has carried out on others also allows you a point of aesthetic comparison or reference: what you consider a beautiful, or natural-looking breast reduction may align more with some surgeons’ work than others. Look closely at the before/after results of patients who share a similar torso and breast shape with you as they offer a fairly good guide to what you can expect.
Check also for consistency—how uniform are the results for the women who’ve undergone breast reduction in the hands of this particular surgeon?
4. A sense of trust or connection with the surgeon
Feeling comfortable with the surgeon you choose and the team supporting him or her represents another critical factor to consider. You will be spending a significant amount of time with this doctor; during the initial consultation period, in surgery, over the course of your immediate recovery and the postoperative follow-up checks that come with them. As such, there could be times when the path may not always be so smooth. A respectful and honest relationship with your surgeon built on a foundation of trust, transparency and respect is a central consideration.
Here are some useful questions you can ask yourself to check how you feel about a potential surgeon:
- Do I feel at ease and comfortable during consultations?
- Do I feel like I can trust him or her to act in my best interests, and do what is right and safe for me?
- Do I feel comfortable asking this surgeon questions throughout the process, particularly awkward ones?
- Do I feel comfortable disclosing my complete medical history and any habits that may impact on my health and safety to this surgeon?
Being able to answer affirmatively to the above questions is vital and shows that you are in the initial stages of developing a healthy trusting relationship with your surgeon.
5. Patient safety in all aspects of surgery
Although breast reduction is a form of elective surgery, it nonetheless carries very real risks if patient safety is not scrupulously upheld. Even if you trust your surgeon and have determined that he or she has board certification and sufficient expertise in reduction mammoplasty, there are other elements of surgery that affect your safety and well-being: for example, the operating facility and the anesthetist.
Ask your surgeon where the surgery will be performed, and if the operating rooms are accredited. Accredited operating facilities have life support systems in the rare event that something goes wrong. Look for AAAASF, AAAHC or JCAHO facility certification.
Also ask about the qualifications of the anesthetist or the anesthesiologist who will be responsible for your sedation during the procedure. The use of anesthesia can present risks and requires careful management tailored to the individual needs of the patient. To have peace of mind about your safety, ask for a Certified Registered Nurse Anesthetist, (CRNA) or a Board Certified Anesthesiologist to administer your anesthesia during surgery.
6. Customer service
Breast reduction can be a costly procedure, and you have the right to expect good service and appropriate treatment that makes you feel valued and comfortable.
When you walk through the doors of a clinic for the first time, pay attention to the following:
- Is the staff friendly and helpful?
- Are you given all the information you need to know in order to make an informed decision?
- Do you feel fully prepared for the possible risks and realities of surgery and recovery?
- Is the total cost clearly stated, with all the contributing elements of the final quote itemized?
- Do you receive prompt and informed replies to your questions?
10 Questions to Ask During Your First Consultation
For many patients, knowing what to ask during the first consultation can be overwhelming or intimidating. Medical discourse can often seem full of jargon and inaccessible to non-medical professionals. However, it’s critical that you ask questions so you are better able to advocate for the results you want and deserve. Engaging with your future surgeon through question and answer sessions can guide you to a better understanding of what surgery entails, any risks or complications that could arise from it, and inform you about the kind of results that can realistically be achieved.
Below is a list of straightforward questions you may wish to ask your surgeon to better inform your decision:
- Are you certified by the American Board of Plastic Surgery?
- Were you specifically trained in the field of plastic surgery?
- Where will my breast reduction procedure be performed?
- What type of breast reduction would you recommend in my case?
- Is the surgical facility where the operation will be performed accredited with AAAASF, AAAHC or JCAHO facility certification?
- Am I a good candidate for breast reduction?
- Are there any specific risks or complications I would face as a result of surgery?
- How will my breasts change over time?
- What happens if I’m dissatisfied with the results?
- Will my breasts change as a result of pregnancy or breastfeeding?
Surgeons appreciate patients who are informed and engaged, as it means they are better able to mitigate risk and complications, care for and manage themselves after surgery, and generally enjoy better outcomes.
How Much Does Breast Reduction Surgery Cost?
According to 2015 statistics released by the American Society of Plastic Surgeons, you should expect to pay $5,425 on average for the procedure (aesthetic patients only). However, breast reduction surgery can cost up to $20,000. Additional expenses that may need to be factored into the final price include:
- Anesthesia/anesthesiologist fees
- Costs of the surgical facility where the operation is being carried out
- Preoperative medical tests
- Post-surgical garments (for comfort while you heal)
- Medication
Costs can also vary widely based on the experience of the surgeon performing the procedure, the type of procedure being carried out, and the geographical location of the office.
Insurance for Breast Reduction
Women with larger breasts are often relieved to hear that the cost of breast reduction can be subsidized or paid in full by their health insurance. Many health insurance plans cover breast reduction surgery so long as the insurer is convinced breast reduction is ‘medically necessary’. The criteria used to determine as much can differ between insurance companies, but all will generally require proof in the form of a letter written by your plastic surgeon, accompanied by photographs from the neck down.
“Patients have to demonstrate that their breasts are large in proportion to their frame and they need medical care because of the size of their breasts — for neck or back pain, rashes under their breasts, chronic headaches or difficulty with physical activity,” says Dr. Kelly Killeen.
However, even if your surgeon determines that you’re a good candidate for reduction surgery based on your figure and medical history, it doesn’t necessarily mean your insurance company will agree to cover the procedure.
According to Dr. Amy S. Colwell, a plastic surgeon based in Boston who specializes in breast surgery, insurance companies generally seek the expertise of a panel of doctors who consider the patient in question in relation to a set of charts that take into account height, weight and the quantity of tissue that can be excised from each breast. In most cases, your surgery will be covered by insurance if the amount of breast tissue to be removed weighs between 1 and 4 pounds. However, standards vary between insurance providers, so it’s important to talk to a company representative to determine the criteria and extent to which your surgery will be covered.
Once authorization to proceed is obtained, you can confidently start scheduling dates for your surgery. You will, of course, still be responsible for any deductibles or contributions required by your insurer.
Reduction Mammoplasty Techniques
Breast reduction surgery is performed through different incision techniques. In some cases, excess breast fat may also be removed through liposuction, either as a complement to surgery or as the sole reduction procedure.
While all surgical breast reduction techniques share the common aim of removing excess glandular, skin and tissue mass, the incision technique selected to do so varies, with different incisions resulting in slightly different outcomes. The technique most appropriate for you will be determined by your surgeon’s expert opinion, your personal preferences, breast composition and the extent of reduction desired.
“For very large breast reductions, over 500 or 600 grams, the anchor shape is best, whereas a lollipop is better for smaller breast reductions between 300 and 500 grams,” explains Dr. David Kulber, director of the Plastic Surgery Center of Excellence at Cedars-Sinai Medical Center. “It’s definitely case-by-case. It depends on scarring versus shape.”
In addition to removing excess breast weight, a breast reduction by nature will include a breast lift (mastopexy) so your breasts sit higher on your chest and appear cosmetically more attractive. Although most women undergo breast reduction to address physical difficulties or issues, there are aesthetic advantages to be gained from the procedure as well.
Anchor Incision Pattern
The anchor incision pattern, commonly referred to as the ‘inverted T’, is the most traditional surgical technique. It consists of three distinct incisions. The first incision is made on the edge of the areola, the second incision takes place in the middle of the breast, and the final incision is made under the inframammary crease of the breast (thus giving the procedure its name, the ‘anchor’ pattern). This incision pattern allows for maximum tissue and skin removal.
This approach is most frequently used for patients with extremely oversized breasts who won’t benefit as much from less invasive methods. Patients with asymmetrical breasts and/or pronounced sagging (breast ptosis) are also candidates for this technique.
Advantages:
- Removal of excess skin relieves moderate to severe breast sagging
- Straightforward cut and reduction technique
- Breasts are tighter and firmer following surgery because of the excision of unnecessary skin and tissue
Disadvantages:
- The “inverted T” incision pattern leaves some scarring in the places where the incisions were made. However, with proper care, scars fade considerably over the first year after surgery, and can be easily concealed by clothing and swimwear.
- The breast size will be reduced, but the breast may appear flatter if not accompanied by reshaping.
- Over time, the breast may droop, looking hollower on top and fuller on the bottom.
Pedicle Method
The pedicle method is a reduction technique which removes excess tissue, but also repositions the nipple, effectively ‘lifting’ the breast. The areola and nipple are relocated to a higher position on the breast to match the new breast shape, but still remain attached to a mound of tissue containing ducts, nerves and blood supply so breast function and sensation is maintained. Pedicle methods may also be used in conjunction with the vertical or anchor incision methods, as well as liposuction.
There are two main variations of the pedicle method.
- The inferior pedicle method: the nipple and areola remain attached to the tissue below the areola while it is repositioned. Of all the pedicle variations, this is the most common procedure. One reason for it’s popularity is because it poses the least risk of losing sensation in the nipple, and also offers women a better chance of being able to breastfeed once they have healed from surgery.
- The superior pedicle method: the nipple and areola remain attached to the tissue above the nipple and areola. The superior pedicle method can offer women perkier cleavage because it removes the hanging tissue on the lower half of the breast. However, some studies have shown that the superior pedicle incision technique has been associated with less plentiful milk production because of the location of the incision, which severs the primary nerve that enables milk release.
There are two other pedicle methods, but they are less commonly used by surgeons: the medial pedicle method, where the nipple and areola remain attached to the inner portion of the areola, and the lateral pedicle method, where the nipple and areola remain attached to the outer portion of the areola.
The pedicle method is most commonly performed on women who have lax, saggy breasts, and will most benefit from repositioning the nipple in conjunction with the removal of excess breast tissue.
Advantages:
- The pedicle method is very safe, with a low likelihood of complications occurring.
- It can be performed without severing blood flow to the nipple.
- The breast function can be maintained.
- The contour and overall appearance of the breast is enhanced.
- The technique is appropriate for a wide range of breast sizes.
Disadvantages:
- Following surgery, the patient is left with a permanent scar around the areola. This will, however, fade over time with proper care and attention.
- Some variations of the pedicle method may impact on nipple sensation.
- Some variations of the pedicle method may impact on milk production.
Vertical Incision Technique (The ‘Lollipop’ Technique)
The ‘lollipop technique’ simultaneously reduces the breast size while reshaping it. The upper portion of the breast that gives the appearance of cleavage is preserved while the hanging lower portion of the breast is removed, creating a lifted, more attractive breast shape.
The vertical incision technique is most commonly carried out on women who only require a moderate reduction in breast size. Two incisions are made during the procedure: one around the periphery of the areola, the other a vertical incision from the bottom of the areola to the breast crease, or inframammary fold.
This incision pattern allows for the removal of modest amounts of excess fat, tissue and skin. The breast is then reshaped internally into a smaller, more compact shape. Liposuction is often used to supplement this incision technique.
Ideal candidates are women with mild to moderate breast sagging with good skin elasticity who do not have a large quantity of excess breast tissue.
Advantages:
- There is less scarring than the other incision techniques.
- Reduced recovery time (you may be able to return to work in one week).
- There is less pain, swelling and bruising.
- The procedure results in a fuller, more natural breast shape.
Disadvantages:
- A vertical scar will be left on the breast, but it’s only noticeable below the breast and nipple and easily concealed beneath a bra or top.
- This surgery is not as effective for women with very large breasts.
Liposuction
In many cases, liposuction may be used as an supplementary method of removing breast fat in conjunction with the techniques described above.
Some surgeons recommend body liposuction simultaneously with breast reduction surgery, particularly for women who’ve had a substantial quantity of breast tissue removed. Liposuction carried out in the vicinity of the breasts can enhance results by trimming excess tissue from underneath the armpit, the upper back, and above the rib area. Slimming around the upper body provides an advantageous setting to help the breasts appear full and natural. Combining liposuction with a breast reduction allows you to enhance your breasts and slim your frame at the same time.
For women whose large breast size is largely due to fatty tissue, liposuction may solely be used for breast reduction. However, very few women meet the criteria necessary to undergo a liposuction-based breast reduction.
Women with moderately sized breasts (limited to DD cup size), good skin elasticity and excellent nipple placement are ideal candidates for this technique.
Advantages:
- Liposuction-based reduction is a far less invasive procedure.
- There is less risk of complication.
- Scars are shorter and less visible.
- Recovery time is much faster.
Disadvantages:
- Achieving optimal results with liposuction can be difficult, because only fatty tissue is removed, not actual breast tissue.
- It is not an effective procedure for women with extremely large breasts.
- Women with nipples which have a lower position on the breast will not benefit from this technique.
- The breasts do not undergo any re-contouring or lifting, and the nipple is not repositioned.
Free Nipple Graft
For women with extremely large breasts (gigantomastia) who undergo breast reduction, sometimes the nipple areola complex must be completely detached from its current location in order to be appropriately relocated in an elevated position when the breasts have been reduced. This method is known as a free nipple graft.
Patient must be aware that the loss of nipple sensation and the ability to breastfeed is possible following this approach.
Preparing for Surgery
Feelings of fear, anxiety or being overwhelmed about your upcoming surgery are entirely normal. Sometimes, an effective way to deal with these emotions is to be pro-active as you wait, taking measures to prepare yourself for surgery so that everything goes as well as it possibly can and your recovery is swift and complication-free.
The Month Before
As the time leading up to your surgery draws closer, it is highly likely that you will be asked to attend a pre-operative appointment. This will allow the surgeon to check that your health is sufficiently robust for the surgery to be carried out.
You may be asked to undergo some of the following tests:
- CBC (Complete blood count): your red and white blood cell levels will be checked to identify any pre-existing conditions such as anemia, lymphoma or leukemia, and determine if your body is fighting an infection.
- PT/PTT blood tests to check your blood clotting/coagulation is normal
- UPT (urine pregnancy test)
- If you are 55 or older, you will also undergo an ECG (electrocardiogram) to check if there are any problems with the electrical activity of your heart.
The doctor may also instruct you to get a mammogram, particularly if you are over 55 years old, to ensure there is no cancerous tissue in the breast prior to surgery. Having preoperative and postoperative mammograms can help create a baseline of your breast health before surgery and note any shifts or changes in your breast that occur as a result of surgery (such as calcifications, scars, masses or lesions).
The surgeon will also provide you with a list of instructions to follow in the weeks leading up to your scheduled surgical date. These instruction lists usually outline the following recommendations:
- If you are a smoker you must cease smoking well in advance of surgery (at least 6 weeks). Smoking increases the risk of necrotic tissue (tissue death) and nipple loss. If you have anxiety about giving up the habit or need support, there are many groups and networks throughout the U.S. that can help you overcome nicotine addiction.
- You will be given a list of medications to avoid, such as aspirin, anti-inflammatory (Motrin, Ibuprofen) drugs and certain herbal supplements as they can thin the blood and cause problems with clotting. If you’re concerned about any medication or supplements you’re currently taking, it’s best to check with your surgeon to see if it’s safe to continue with them.
- Eat a well-balanced, wholesome diet. Increase your intake of unrefined foods, leafy greens, fresh seasonal fruits and vegetables and whole grains, and reduce your intake of starchy foods, highly processed junk foods and sugar. Ensure you avoid over-consumption of salty foods, as salt causes the body to retain the water and swell. Also have nutritious, easy to eat snack foods on hand for the recovery period: raw vegetables, nuts, wholegrain crackers and fruit.

RELATED: Your Pre- and Post-Surgery Diet
The Week Before
Freeing up your schedule in the days before your breast reduction will give you time to prepare yourself for the surgery and recovery period that will follow.
- Purchase any antibiotics, medication or over the counter prescriptions that you have been recommended for your recovery. Surgeons often advise purchasing Dial Antibacterial or Hibiclens soaps as well to keep the surgical site clean.
- Delegate responsibilities so you are not faced with stress leading up to surgery—call on support people to help you manage childcare, pet care, cooking and cleaning so you can be free from stress while you’re getting ready for surgery and recovering.
- Start taking time for yourself to relax: take baths, walks, practise yoga or gentle physical activities, watch a film. Feeling relaxed and rested can help immensely before going into surgery.
The Day Before
Your surgeon is likely to give you specific instructions about what you need to do in the hours leading up to your procedure.
- Remove any nail or shellac polish (unless it is clear) and acrylic nails. During surgery you will have a device clipped onto one of your fingertips that measures the oxygen saturation of your hemoglobin. Colored polish and artificial nails can interfere with the readings.
- Wash your hair. Following breast reduction surgery, proper showering will be difficult. Going into surgery with freshly washed hair can be a mood booster. Make sure, however, that it’s dry before you go to the hospital.
- Shower and wash thoroughly, but don’t apply any lotions, creams, moisturizers or deodorants to your skin. Some surgeons may recommend that you prepare for surgery by washing with an antibacterial soap to remove any bacteria from the skin before the operation.
- You will be given instructions about when to stop eating or drinking before surgery (pre-operative fasting). If your surgery is in the morning, you will generally be instructed not to eat anything after midnight and cease drinking water or clear liquids two hours before your surgery. It’s vital to follow these instructions closely as even a trace of food in the stomach can pose a serious risk when your body is under anesthesia, because the gag reflex is relaxed.
The Day of Surgery: What to Expect
Nerves are totally normal on the day of surgery. One of the best ways to alleviate any pre-surgery jitters is to arrive at the facility where your surgery is being performed with plenty of time to spare. This gives you a chance to go through the admittance procedures and settle in without being rushed.
Once you’ve changed into your surgical gown it’s standard practice for the anesthesiologist (or one of their assistants) to do a last minute medical check (concerning your medical history, for example) and for the surgeon to meet with you, review the procedure, and answer any final pre-surgery queries you may have. He or she will likely also make-pre-operative markings on your body to guide where the incisions will be made.
Surgery can take between two and five hours, and will proceed according to the following steps:
1. Anesthesia
All breast reduction surgery will take place under a general anesthetic or intravenous sedation (sometimes referred to as “twilight sleep”). Your surgeon will discuss the option that is most appropriate for you prior to surgery.
2. Incision
Incisions will be made according to the technique discussed in your earlier consultation (pedicle, ‘lollipop’ incision or ‘anchor’ incisions).
3. Excision of breast tissue
The excess tissue is removed through the incision sites, and in some procedures, excess skin will be removed as well. If you are undergoing the pedicle incision method, the nipple mound (while still tethered to its original blood and nerve supply) will be repositioned higher on the breast. The breast tissue will be lifted and shaped.
4. Suturing the incisions
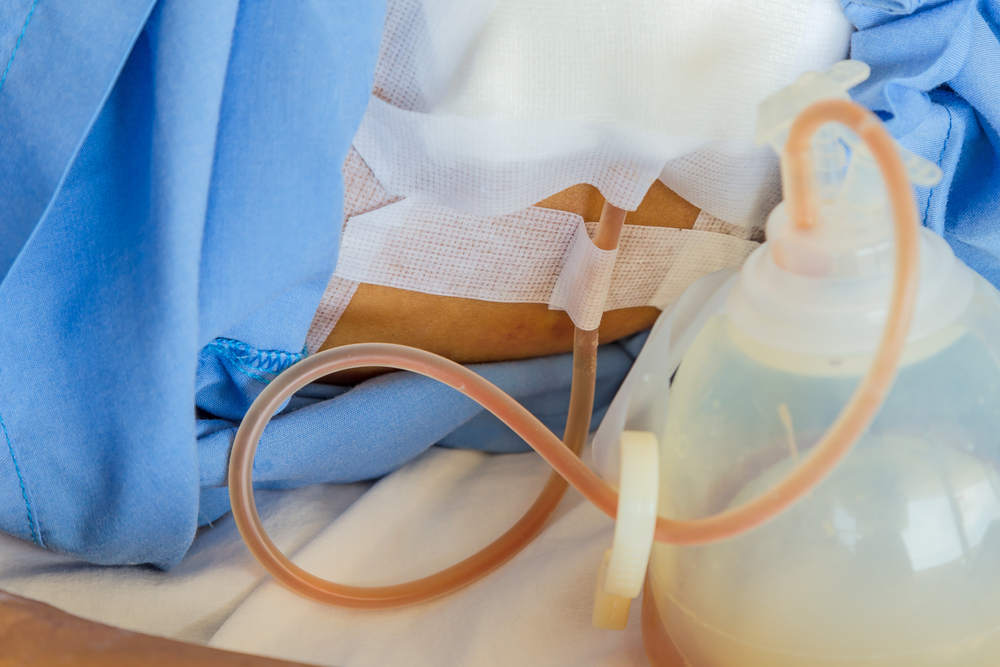
The incisions will be stitched, and the stitches will deeply permeate the breast skin to support and hold the new breasts in shape. Skin adhesives and/or surgical tape will be placed over the sutures. Your breasts will be wrapped in a special gauze, and you may have drainage tubes in place to drain away any excess fluid from the incision site.
Following surgery you will be wheeled into a recovery facility for a few hours to awaken from the anesthesia, closely supervised by staff to ensure there are no immediate complications. Your nurse will follow your specific care instructions as provided by your surgeon, and your recovery will be closely monitored. When your anesthesiologist and surgeon are satisfied you are fully awake and in a stable state of recovery, you will be released to either go home or to an aftercare facility.
The surgeon will then discuss your results and outline post-operative care instructions to adhere to, explaining how to change your bandages, empty your drains (if you have drains), and care for the incision sites.
Breast Reduction Recovery Timeline
Recovery from breast reduction surgery is an ongoing process that occurs in stages. Knowing what to expect and how to properly care for your body as it moves through each stage of recovery will help you to feel prepared, heal and return to everyday life more quickly.
The First Few Days After Surgery
After surgery, you will most probably feel weak and experience mild discomfort in your breast area. Although you may need pain relievers for a week or two, you can expect to feel better and stronger in a matter of days.
Here is a general overview of what you should expect in the days immediately following your breast lift operation.
Bruising (hematoma): Some women may experience bruising following surgery. The extent of bruising depends on the patient and the breast reduction technique. If you are bruised, rest assured that this normally subsides within a week.
Ask your surgeon for advice about treatments such as Bromelain or Vitamin A to help dispel bruising more efficiently. Warm compresses applied to the bruised area several days after your surgery can also help dilate the superficial blood vessels, but always check with your surgeon first.
Swelling (edema): For the first few days following your reduction procedure, you should expect to feel swollen. Swelling is a natural inflammatory response to injury, with fluids rich in hemoglobin and and white blood cells gathering at the wound site to facilitate healing.
If you experience severe swelling, however, it could be indicative of something more serious, so seek medical advice.
Surgical bra/dressing: Post-operative breast reduction patients are commonly requested to wear a surgical bra, elastic bandages or a sports bra that zips open at the front to hold the breasts in place following surgery.
These garments may feel a little uncomfortable but are important as they offer support to your new breasts and can drastically speed up the recovery process by reducing swelling.
Caring for the incision sites: One of your most important responsibilities in the immediate period following surgery is to keep the incision sites clean and dry. Your surgeon may place Steri-Strips on top of your incision sutures to protect them, or you may have an external tissue glue that binds the edges of your incisions.
The surgeon will provide you with details about caring for the incisions to best facilitate healing. It’s important to avoid getting the site wet or placing any creams, salves or lotions nearby as they can provoke inflammation. Most patients are provided with antibiotics to decrease the risk of infection. Make sure you take the antibiotics as prescribed.
Postoperative follow-up appointment: Your first follow-up will occur one to two days after surgery and give your surgeon a chance to remove any drains attached to the incision sites and assess your recovery. The incision sites will also be checked.
Self-monitoring: Patients are encouraged to be vigilant about monitoring their health following surgery. Keeping an eye on your temperature and making sure your pain is under control is vital to ensuring your recovery is free of complications. Feelings of tenderness, stiffness and soreness for the first few days following surgery are normal and to be expected.
You can mitigate these feelings by taking the pain relief prescribed by your surgeon. Keeping pain at bay is better for your overall experience and also quickens your recovery time. There’s no reason to suffer as you heal, so regular (but not excessive) use of pain relief medication is advised.
Some patients are offered the option of a pain pump, which delivers targeted pain relief directly to the surgical site with the added benefit of no grogginess, which is often a side effect of oral pain relief. However, not all surgeons offer the use of pain pumps, and those that do will add it as an extra expense to your final bill.
Checking your temperature regularly is also important as it provides feedback about your body as it heals. An elevated temperature could be a symptom of an infection. Noting any changes in temperature early allows you to respond more quickly and seek medical advice before the situation escalates into something potentially serious.
Activity: Although you may not feel like it, walking and moving around gently is important to get blood flowing throughout your body. Lying down for extended periods of time heightens the risk of blood clots occurring, and makes swelling take longer to dissipate. Strenuous or vigorous exercise at this stage of recovery is discouraged, however.
Sleeping: Surgeons strongly recommend sleeping in a position that elevates your torso to relieve pressure around the breasts and minimize swelling and pain. Sleeping in an elevated position can be challenging, so your surgeon may prescribe medication to help you sleep more easily. Placing a cushion under your knees and alongside your body can also help you to maintain an upright position and feel more comfortable.
Bathing: Showers and baths are off limits until your stitches have been removed. You will need to take sponge baths for the first few days after surgery. Try to avoid washing your hair by keeping it neatly tied back or braided. If you must wash your hair, ask a friend or loved one to help you. Dry shampoo can be a savior, giving the appearance of clean hair without the need for water or rinsing.
1-2 Weeks After Surgery
By now you should feel considerably better, and may even be back at work. However, some bruising and swelling may remain apparent for several more days.
Suture removal: Your stitches will be removed approximately ten days after surgery. Some women find suture removal a little painful, but rest assured it is a quick process and any discomfort will be momentary. The feeling of stitches being removed has been likened to a tugging sensation accompanied by some stinging.
One of the best things about stitch removal is that it means you can take showers, wash your hair and bathe normally again.
Work: Most women return to work and everyday life within 1 to 2 weeks of their surgery. That said, it’s essential to take all the time you need to give your body the chance to rest and recuperate. Some patients may need a little more time before they feel ready to resume work.
Physical activity: Gentle sustained exercise is recommended at this stage of recovery. Brief walks are ideal. It is still advisable to avoid strenuous exercise as it can raise your blood pressure and cause bleeding.
3-4 Weeks After Surgery
By now, most of your swelling should have subsided and your final breast shape should be apparent. Some minor swelling may persist for 3 to 4 months, although this will not be noticeable to anyone but you. Regular fluid intake, a reduced sodium diet and regular exercise all help to mitigate any lingering swelling.
At this stage of recovery you can think about returning to your regular exercise routine if you feel ready and your surgeon approves. Weights, cardio and more vigorous training regimes can be resumed.
RELATED: How to Minimize the Appearance of Surgical Scars
Risks and Complications
Similar to any invasive surgical procedure that requires anesthesia, breast reduction surgery does pose some risks. Fortunately, serious complications arising as a result of surgery are rare, and risks can be minimized by closely adhering to your surgeon’s pre-operative and postoperative instructions.
As Dr. Kelly Killeen emphasizes, “Most complications that happen with breast reduction are minor things, not major complications that land you in a hospital.”
Nonetheless, certain patients face a higher risk or likelihood of complications occurring than others. Many women who require breast reduction surgery suffer from obesity and as such are more susceptible to heart disease and diabetes, heightening the risk of complications like a postoperative wound infection, or blood clots occurring.
One study from 2011 reviewed 1192 patients who had undergone breast reduction surgery and found the likelihood of postoperative risk increased among women aged 50 and older. These patients experienced a higher risk of poor wound healing and infection. The authors of the study argued that this was due to lower estrogen levels impacting on healing. Older women on hormone replacement therapy fared better, however.
Some complications that may occur following surgery include:
- Hematoma or bruising: a collection of blood build-up as a result of internal hemorrhaging within the breast
- Seroma — a pocket of fluid build-up beneath the breast skin
- Infection: abscesses, pus or excessive swelling may be symptomatic of an infection
- Bleeding around the incision sites that does not cease
- Permanent bruising, or discoloration around the breasts that persists for several months following your operation
- Allergic reactions: allergies may occur as a reaction to the anesthesia, surgical dressings, bandages or suture tapes or adhesives
- Unsatisfactory results that require revision surgery
- Breast asymmetry: one breast appears larger or smaller, or hangs lower than the other
- Blood clots in the legs or lungs
- Nerve damage in the nipple or parts of the breast: you may experience burning or prickling sensations, tickling, or numbness as the nerve heals and returns to its normal function. In rare cases, however, nerve damage is permanent.
- Nipple over-sensitivity resulting in constantly erect, sore nipples
- Necrosis of nipple skin necessitating nipple removal and reconstruction
- Trouble breast feeding
- Raised red scars known as keloids
At the first sign of any of the above complications occurring, immediately contact your surgeon or seek medical advice.
Results and Satisfaction Rates
As soon as the bandages are removed your results will be visible. Your new breast size will allow you to enjoy all the physical activities you’ve always wanted to partake in but couldn’t before, and will also enhance your self-confidence.
One study conducted in 1999 and published in the British Journal of Plastic Surgery demonstrated that women who’d undergone breast reduction self-reported an improvement in health status and psychological functioning, with improved body image and body satisfaction and decreased anxiety and depression levels.
However, it may take several months for your breasts to settle into their new shape: they may appear flat, high and slightly unnatural-looking at first but will drop and soften as the swelling subsides and your skin relaxes. It’s also important to remember that although there will always be some scarring, you can greatly diminish the appearance of scars by applying topical oils or creams like Vitamin E.
The results of a breast reduction are permanent. Some changes or fluctuations may occur in the shape and size of your breasts if you gain or lose a significant amount of weight, go through menopause, or become pregnant. Over time, you can also expect the natural effects of ageing and gravity to cause your breasts to loosen and sag.
Maintaining a relationship with your surgeon and returning for follow-ups or evaluations at prescribed times will help ensure you maintain beautiful, healthy results.
Frequently Asked Questions
What is the best age to undergo breast reduction?
As a general rule, it is best to undergo surgery when you are young. Carrying out surgery when you are younger is desirable as it means you can enjoy a normal life and physical activities sooner, without having to endure ongoing back or neck pain because of the heaviness of your breasts.
If you undergo reduction mammoplasty and are aged fifty or older, the chance of complications occurring increases. However, if you’re in good health with no pre-existing medical conditions then breast reduction could still be right for you.
How is the extent of my reduction decided?
Your surgeon will make a recommendation for you based on your needs, goals and desired outcome. Anywhere between 300 to 1300 grams may be removed.
You should be aware that if your health insurance agrees to pay for your surgery then you are subject to their recommendations. It is possible that they recommend the excision of more breast tissue than your surgeon, leaving you with less breast tissue than you would like, or forced to cover the cost of the procedure should you disagree with their recommendation.
Which reduction technique is right for me?
There are a range of incision patterns used by surgeons to excise unwanted breast tissue and reposition the nipple areola complex. The inferior pedicle method and “lollipop technique” are popular for women who want reduction with some reshaping. The anchor incision method is an effective technique for women with larger breasts who need more tissue removed. In some cases, the surgeon may be able to reduce your breast size with liposuction alone.
When you consult with your surgeon, he or she will outline the technique that will provide the best outcome for you.
Will breast reduction surgery impact my ability to breastfeed?
While surgeons take every care to avoid damage to the nipple and areola complex, procedures that involve repositioning the nipple carry a higher likelihood that breast feeding in the future could be affected.
If you have extremely large breasts and require a free nipple graft (complete removal of the nipple to a higher position on the breast following reduction) there’s a heightened chance you’ll be unable to breastfeed in the future because nerves and milk ducts will have been severed from the nipple.
Talking to your surgeon about your ability to breastfeed based on which technique you undergo is essential.
Will insurance pay for my surgery?
Insurance will cover the costs of breast reduction surgery if you meet their criteria (they often have a panel of medical experts who determine your eligibility for surgery based on your height, weight, breast weight, and other factors). You’ll also need a letter from your surgeon explaining why you are a good candidate, and photos from the neck down.