Since the first silicone breast implant surgery was first performed on a young Texas housewife in 1962, millions of women have opted to increase the size of their breasts. Breast augmentation surgery allows women to augment their cup size, and as a result, enjoy feeling feminine and empowered in their bodies.
Updated, August 2017
What You Should Know Before Undergoing Breast Augmentation
Breast augmentation — also known as augmentation mammoplasty — is a surgical procedure that can be used to correct the size, shape, symmetry, and other aspects of a woman’s breasts. It’s the most popular cosmetic surgical procedure in the United States, with 305,856 procedures performed in 2015, according to the American Society of Aesthetic Plastic Surgery (ASAPS).
There are several reasons why this procedure is so popular. Breast augmentations are often performed for medical reasons, such as micromastia (underdeveloped breasts), mastectomy (removing breast tissue), and significant asymmetry (most women have one breast that is larger than the other), but more commonly, they’re carried out for emotional or aesthetic reasons.
Breast implants can replace volume and fullness after weight loss or pregnancy, or help boost confidence. Some women undergo augmentation to improve their sex lives or to gain a competitive edge in their career, while others simply desire a cleavage that fits clothes better.
Deciding to pursue breast augmentation is an entirely personal and private decision. Women should not feel ashamed or embarrassed because of this procedure — it’s not vain or shallow to want bigger or ‘different’ breasts.
That said, making the decision shouldn’t be taken lightly. Breast augmentation is major surgery that includes risks, side effects, and requires significant recovery. If you do decide to pursue breast augmentation surgery, one of the most important decisions you will make is selecting the right surgeon.
Choosing the Right Surgeon
Breast augmentation is as much of an art as it is a medical procedure with different techniques, options, and variations that surgeons can use to deliver the desired outcome. The methods each surgeon uses will depend on a variety of factors, including the patient’s budget, age, and aesthetic goals. Selecting the right plastic surgeon to perform your breast augmentation is absolutely crucial.
1. Find a board certified plastic surgeon
All plastic surgeons are cosmetic surgeons, but not all cosmetic surgeons are plastic surgeons. If you’re looking for someone to perform a breast augmentation, look for a surgeon certified by the American Board of Plastic Surgery, or if you are in Canada, ensure your surgeon is certified by the Royal College of Physicians and Surgeons of Canada (RCSC).
Board certification is important because it helps ensure that a physician has demonstrated competence in his medical specialty, maintains good standing within the healthcare community, stays up-to-date and current scientific findings in their field, and acquires new skills to improve patient outcomes.
There are three certifications that you should pay attention to when it comes searching for a qualified surgeon to perform your breast augmentation: American Board of Plastic Surgery, the American Society of Plastic Surgeons (ASPS), and the American Society for Aesthetic Plastic Surgery (ASAPS).
2. Referrals
Many patients use word-of-mouth to begin their search for a surgeon. If you know friends or family members who have enjoyed excellent outcomes from breast augmentation surgery and recommend a particular surgeon, this can be a useful way to make a connection with a potential doctor. Do ensure, however, that you check the credentials/ board certification of any surgeons you are referred to.
3. Check the facilities where the surgeon operates
Board certified plastic surgeons are required to perform their surgeries in an accredited ambulatory facility with licensed medical professionals, such as anesthesiologists and registered nurses. There are four accrediting bodies that verify such operating facilities safety:
- Accreditation Association for Ambulatory Health Care (AAAHC)
- The Joint Commission
- Medicare
- American Association for Accreditation of Ambulatory Surgical Facilities (AAAASF)
According to the American Society for Aesthetic Plastic Surgery, “current published data show that accredited office-based facilities have a safety record comparable to that of hospital ambulatory surgery settings.” However, the majority of office-based surgical facilities are not accredited.
4. Follow up care
Post surgical care is an important part of your breast augmentation, and it is important to be able to schedule and attend follow-up appointments to monitor healing and watch for signs of infection or adverse events. For this reason, it is advisable that patients select a physician within a reasonable commuting distance.
5. Rapport
Many women are advised to “go with their gut” when it comes to choosing a care provider, but what does this advice mean? It means being comfortable to be open and honest with the surgeon about every aspect of your health and the surgery.
With a good rapport, patients are more comfortable sharing health concerns and alerting staff of potential problems with recovery. They are also more willing to follow a doctor’s advice is they trust and like them, which goes a long way towards a speedy recovery.
RELATED: How to Find a Plastic Surgeon You Can Trust
Your First Consultation: Questions to Ask
After you’ve created a list of plastic surgeons to consult for your breast augmentation, you will need to schedule an initial consultation. The consultation is a chance for the patient to meet with the surgeon who will perform the surgery, ask the doctor questions and receive their professional opinion on implant type, size, and surgical techniques, and assess your rapport.
Consultations are performed in the surgeon’s office, although many offer online consultations that may better suit a patient’s schedule. Many plastic surgeons charge a non-refundable consultation fee averaging $100 for a 30-minute consultation that can be applied to the cost of the procedure. However, some doctors do not charge this fee, and the presence or absence of a fee isn’t always an indicator of their skill.
For the initial consultation, many patients bring their medical records and photos of their ideal breast augmentation results. Examples of questions often asked by patients at this time include:
- Are you board certified?
- In what states are you licensed?
- In what hospitals do you have admitting privileges?
- What is the most common operation you perform?
- How long have you been performing breast augmentations?
- How many breast augmentations have you performed?
- What are some complications that you have encountered during surgery?
- Is the facility where the surgery will be performed an accredited ambulatory facility?
- What is the procedure if you experience a complication during surgery?
- What support do you offer pre- and post-surgery to ensure optimal results?
- What happens if I am not happy with the outcome of surgery?
As part of the consultation, patients should expect the doctor to perform a brief medical exam to review their current health and inquire about their medical history. The surgeon may assess your breasts for:
- Size, shape, and symmetry
- Proportionality to your body
- Quantity, quality, and density of breast tissue
- Nipple placement
- Skin laxity and thickness
- Ptosis (sagging)
- Placement on the chest wall
- Breast and width
- Incision options
Your surgeon may also wish to find out about:
- Your current medical condition
- Your medical history
- History and experience with prior surgeries
- Family medical history, including incidences of breast cancer
- Mammogram results
- Your aesthetic goals
- Your exercise routines
- Your mental health and stress levels
Breast Augmentation Simulators
Technology is changing the way women research their breast augmentation. These advances are going beyond finding just the names and addresses of doctors – today they can be used to help women interview potential surgeons and get quotes without leaving the house, and computers are making it easier for women to visualize the size and shape of proposed implants.
Illusio
Illusio 3D gives patients a chance to see what breast implants would look like on their body post surgery. Illusio 3D uses an iPad like a virtual mirror that enables the patient to examine the proposed implant on her body from all angles.
By superimposing the augmented breasts onto the woman’s frame, she can get a better sense of what the size looks like in proportion to her body, and ensure that she and her surgeon are in agreement on shape and size.
Crisalix
Patients can access the same 3D imaging tools that plastic surgeons use to show their patients what future results could look after the surgical procedure. This fee-based service enables patients to upload a photo to Crisalix’s secure site and alter the image to see how cosmetic procedures would look on their face or body.
Virtual Reality
Some offices are combining technologies such as Axis Three (shown below) and Vectra 3D with cutting edge hardware to create a virtual reality experience for trying on a new breast size.
Using Virtual Reality glasses such as Oculus Rift, patients will be able to walk around 3D simulations of their body to see from all angles what they would look like after a breast augmentation, breast reduction, or breast lift.
Types of Breast Implants and Enhancement Techniques
Implant size is the just the start of the many decisions you will need to make for your surgery.
You will need to decide on the type, texture, shape, size, placement, and surgical incision of your implants – that is if you decide on an implant in the first place. These days, many women are opting to use their own body fat — also know as autologous fat transfer — to increase their bust size.
But first things first, what are your implant options? Here is some information on the types of implants available to help you make your decision.
Saline Implants
Saline implants are silicone shells that are filled with saline (salt water). Although they are not as popular as silicone implants, they have many benefits, including that they can be inserted through small surgical incisions and filled to a large volume. Saline implants are also the only FDA-approved implant for patients younger than 22 years old.
However, they are more prone to ripples that are visible under the skin (even if they are placed under the muscle), and may be more vulnerable to leaking, leading to deflated breasts that requires revision surgery or repair. On the upside, when there is a leak, you will notice immediately. On the downside, when a rupture occurs — a problem that can occur with silicone gel implants as well — you will need to repair the implant quickly.
Another benefit is that they are usually less expensive than silicone implants, but they may not feel as natural.
Silicone Implants
Silicon implants were first used in 1962, and were approved by the FDA for cosmetic surgery in 1996. Prior to that, they were approved only for reconstructive surgeries and revision. In 2015 they were used in 85% of all breast augmentations.
Silicone implants are filled with a thick, gooey silicone gel that is viscous. Many patients find that silicone implants feel the closest to their natural breast tissue. However, they are more expensive than saline implants and depending on the size you aim for, may limit the incision options. Although silicone gel isn’t liquid, it may still leak, show ripples, or require replacement.
Generally, silicone implants last 10 years, although in many cases they will last longer, and are longer-lasting than saline implants. There is a wide range of silicone options, including round, oval, smooth, or textured implants.
Extensive studies have been conducted and there is no conclusive evidence that silicone breast implants cause cancer. However, silicone implants may make it harder to detect tumors during mammogram, which can delay cancer diagnosis.
- Round cohesive silicone implants
This popular style of implant is used by physicians because it provides a “upper pole” volume in the upper aspect of the breast, comes in a range of sizes, and can be smooth or textured. Women report that silicone implants have the most natural feel. As they are symmetrical, it is not noticeable if they rotate within the body.
- Anatomic (shaped) cohesive silicone implants
To achieve a particular shape or profile of the breast, a surgeon may recommend a shaped silicone implant. Shape options include oval, wide base, and high profile. However, they are more noticeable if they shift or rotate, and often require a larger incision.
- Highly cohesive silicone implants (gummy bear)
The consistency of a highly cohesive silicone implant is firmer than a traditional silicone implants, which is why they are sometimes generally referred to as “gummy bear implants.”
Gummy bear implants are molded to resemble the natural shape of a woman’s breast. The benefit of this implant style is that they are the least prone to leaking, last longer, and will give a more natural shape to women who have lost a significant amount of breast tissue due to a mastectomy.
However, shifting or rotation of shaped implants is very noticeable and requires surgical revision to correct. Women may also find that molded implants don’t move or feel like natural breasts — especially when they are lying down — and may be more uncomfortable during sleep.
- Smooth surface
Traditional implants have smooth surfaces that enable them to move around under the skin or muscle, which creates a more natural look and feel. However, this also can lead to displacement, which requires breast revision to repair.
- Textured surface
The intention of a textured surface is to render it easier for the implant to adhere to the body, which prevents it from shifting, rotating, and moving around. With a textured surface, a natural fibrous capsulation may more easily form around the implant, and there is some evidence that this lowers the risk of capsular contraction. However, in some cases women may find that the textured surface makes the implant more palpable.
Breast Augmentation with a Breast Lift
There are many reasons that women may have breasts that sag, such as weight loss, pregnancy, genetics, or age. For some women, an implant may provide a subtle lift, but for others, a breast lift will be required to achieve appropriate nipple placement.
A breast augmentation with a breast lift represents two surgical procedures, and may increase the cost, scarring, recovery time, and surgical risks depending on the type of incision and technique the surgeon uses to lift the breast. To determine you would benefit from a breast lift in addition to breast implants, a doctor will examine the amount of ptosis (sagging) based on the position of the nipple and its distance from the collarbone.
Fat Grafting Breast Augmentation
An alternative to using silicone or saline implants to enlarge breast size is to use the patient’s own fat. 18,135 fat grafting procedures to the breast were performed in 2015, according to the American Society for Aesthetic Plastic Surgery.
‘Fat transfer’ or ‘fat grafting’ breast augmentations are a two-step process. With this procedure, the surgeon harvests fat from other areas of the patient’s body — typically the love handles, buttocks, or thighs — purifies the fat on site, and then re-injects it into the woman’s breast to create a larger or more balanced shape.
As with implants, this technique has benefits and drawbacks. With fat grafting, there are no concerns about ruptures, leaks, rotation, or capsulation, and many women like the idea of using their own fat rather than a foreign object in their body. However, fat necrosis, or death of the fatty tissue, is a known side effect, and physicians can’t predict how much fat will survive the transfer.
Studies have shown that as much as 20-30% of transferred fat dies after the breast augmentation. As a result, some women may end up with breasts of different sizes and may need additional liposuction and revision surgeries to correct the imbalance.
There is also some concern that fat may harden and form cysts, which can interfere with mammogram readings at a later date. A limitation to this procedure is that typically breasts can be enlarged by only one cup size. This means that if a woman wants to increase her breasts by more than one cup, they would derive more benefits from using implants, or perhaps a combination of the two techniques.

RELATED: Which Looks and Feels the Most Natural — Fat Grafting or Breast Implants?
Choosing a Size for Your New Breasts
Selecting the size of your breasts can represent one of the more gratifying aspects of your augmentation surgery, but it is also daunting. For many women, it can be hard to select a size that achieves their desired increase, yet is appropriate for their body frame, and looks natural.
At the same time, there are many women and doctors who prefer a “surgical” look that is full and bouncy. There is no empirical scale for selecting the correct size, but women should take a variety of factors into consideration, such as:
- Age: Women tend to want larger breasts when they are young, but find when they are older that they prefer a more modest size. Not every woman feels this way, but breast sagging and career trajectories often contribute to this change of mind.
- Clothing preferences: Women’s clothing is typically designed to fit a C-cup. Large implant sizes may make a woman look great in lingerie or bikinis, but they can also limit the clothing options, such as button down shirts or strapless dresses.
- Their activity levels: Large breast implants may interfere with some sports and fitness activities, and the weight may cause back pain in some patients.
- Future pregnancies: Breast size may change with pregnancy.
- Weight stability: Weight gain or weight loss will affect breast size.
Interestingly, the average size of breast implants varies depending on the region, ranging from 250cc to 350cc in the more conservative Northeastern states to 350cc to 450cc along the sunnier West Coast. Overall, the average volume is 390cc, according to a survey of 225 patients by the American Society of Plastic Surgeons.
For the average woman hoping to achieve a full C-cup, most surgeons will use 300cc implants. However, the size of implant used may vary depending on the patient’s frame, chest width, breast diameter, and skin laxity, and the profile and shape of the implant.
Most doctors advise women not to be fixated on cup size because of the variation between bra styles and manufacturers. Furthermore, each patient’s muscular structure is different and will affect how an implant looks.
Getting a breast augmentation is likely to be the first of several surgeries to maintain your implants. Implants have an average lifespan of 10 years — although many last several years longer and need to be monitored regularly to ensure their integrity and check for leaks. It’s likely that one or both will need to be replaced over your lifetime, and many women decide to change sizes down the line.
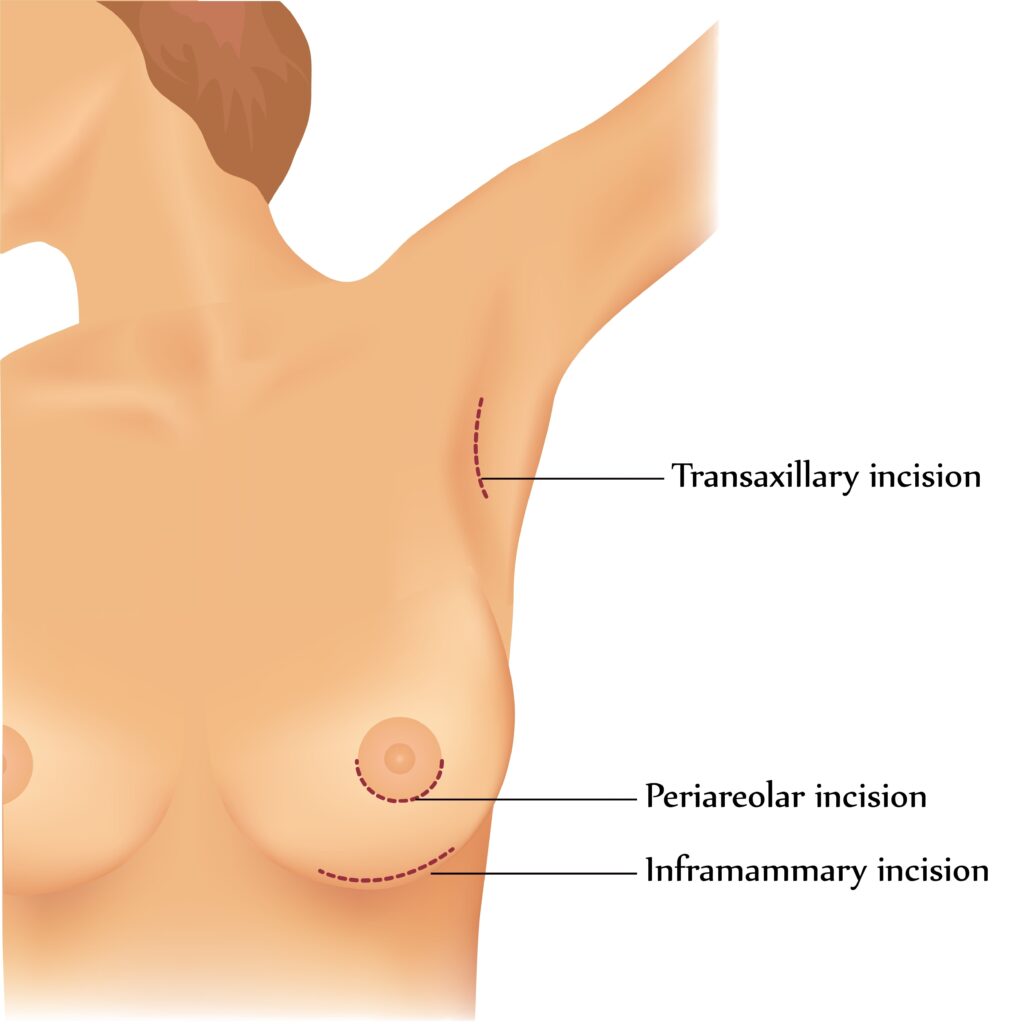
Breast Implant Incisions and Placement
There are a number of incisions that surgeons use to insert breast implants. The size of the implant will also affect the type of incision used.
- Transumbilical: The incision is made around the navel, and the surgeon guides the implant under the skin into position in the capsule pocket. The benefit of this incision is that there is no scarring on or anywhere near the breast, but it is the most difficult for doctor to perform as it makes optimal placement challenging.
- Periareolar: An incision is made around the areola, and the implant is inserted through the nipple. However, incisions around the areola present a small risk of damaging the ducts and glands and may hinder your ability to breastfeed, or cause loss of nipple sensation.
- Transaxillary: the incision is made in the armpit. This position enables the surgeon to fit most implant types (but not very large sizes) into the breast pocket. However, it leaves a short scar that is mostly hidden from view. It is often chosen by women who don’t have a breast crease to hide the scar, but a transaxillary incision can make placing the implant more challenging for the surgeon, still presents a risk of nipple sensation loss, and the scar may be visible in some outfits and arm positions.
- Inframammary: The incision is made under the breast along the fold, and is the most common technique used to insert breast implants. This incision enables the surgeon to have full access to the breast to create the best implant pocket. However, a small scar may be visible when lying flat, although for many women it heals so well that it is nearly invisible. One benefit is that in most cases, neither breast tissue nor ducts are cut, reducing the risk of nipple sensation loss.
Clearly, there are benefits and drawbacks of each type of incision. The good news is that only 1 percent of patients surveyed by the ASPS expressed dissatisfaction with their scars, which were usually located in the crease under the breast.
Over vs. Under the Muscle
There are only two choices when it comes to placing the implant in your body — over the breast muscle, or under it.
Placing the implant over the breast muscle is the easier of the two choices, is less painful, and has a shorter recovery time. However, unless you have a lot of existing breast tissue to cover the implant or are comfortable with the occasionally witnessing a visible ripple, placing it under the muscle is usually the recommended choice.
Implants placed under the muscle tend to look more natural and make interpreting mammograms easier for physicians. However, because the muscle is on top of the implant, compression caused by flexing may occasionally distort the breast shape. In some cases, submuscular placement may cause the implant to “bottom out.”
Preparing for Surgery
Choosing the right breast implants and surgeon goes a long way towards an ideal outcome, but your health also contributes to good results. In the days before surgery you will be asked to:
- Stop drinking alcohol. Many surgeons recommend that patients avoid alcohol several days before surgery to reduce the risk of bleeding due to its natural blood thinning effects.
- Stop smoking two weeks before surgery. Smoking can reduce your blood circulation, which can affect healing.
- Stop medications/supplements that can increase your risk of bleeding. This includes many herbal supplements such as St John’s Wort that can thin the blood or may impact on anesthesia.
- Shower with antibacterial soap for three days prior to surgery.
- Prepare your home for postoperative care: lay out your clothing, cook easy to digest and eat foods, and put all recovery items within easy reach.
- Arrange childcare for a few days following your procedure, and prepare your children for your physical restrictions, such as refraining from picking them up, carrying them, vigorous play, or big hugs.
Breast augmentation surgery is a relatively straightforward procedure — the actual operation only takes one or two hours, according to the ASAPS, and can be performed under local or general anesthesia. However, for the patient’s safety it is almost always performed under general anesthesia.
Here are some pre-op instructions to remember on the day of your surgery:
- You’ll want to take a shower before the procedure, and wash your hair as normal — lifting your arms above your head will be verboten for several days after surgery. Per doctor’s orders, avoid deodorant, perfumes, and body lotions.
- Most surgeons will ask you not to eat or drink anything after midnight so your stomach is empty when you go under anesthesia. Expect to feel hungry!
- Dress in comfortable clothing that is easy to take on and off by yourself with minimal effort, such as sweatshirts with zippers.
- Before you leave for your appointment, ready your room for recovery by placing everything you need within arm’s reach, like food, water, pain medications, and television remotes.
- After you check in for your surgery, you may still have a few hours to wait before your operation. If you’re nervous, your doctor may give you a sedative as you wait for the procedure to begin.
Breast Augmentation Recovery and Post-Surgical Care
Waking up after your surgery is just the start of your journey on the long road to recovery. Your doctor will explain the postoperative care procedure, but here is what you can expect.
- Swelling: What you see immediately after the surgery is not what you will end up with — swelling will make your breasts appear much larger than anticipated and they will “ride high” for several weeks or months until they fall into place. The swelling will subside within three to four months, although you probably won’t know your final bra size for sure until six months after the bandages come off.
- Pain: Most women who have undergone breast augmentation will tell you that the surgery was more painful than they expected, not to mention the stiffness and the bruising. For this reason, it’s a good idea to fill your prescription for pain relief prior to the procedure.
- Drainage tubes: Depending on the surgeon’s preferences and experience, drainage tubes may be used to reduce the risk of fluid build up around the implant to prevent a capsule from forming. Many surgeons do not use them because they can introduce bacteria. However, inflammation from bacteria and fluid buildup both have been proven to increase the risk of capsular contracture.
- Extended recovery time: After 24 hours, you will be able to resume everyday activities, and return to work within three to seven days. But the swelling and discomfort will remain for weeks, and your activities will be restricted. For example, you won’t be able to sleep on your stomach or exercise vigorously for several weeks.
- Loose clothing: Loose tank tops, zippered sweat shirts, and button-up blouses are recommended for your post-surgical wardrobe. However, any item of clothing that you can put on and take off without raising your arms or making an exaggerated movement is recommended. You will have a postoperative garment or sports bra that zips at the front to provide your new breasts with support.
- No alcohol: Abstain from drinking for at least two weeks after surgery to minimize the risk of bleeding and promote healing of your wounds.
- Difficulty showering: Lifting your arms to wash your hair, bending down to wash your feet, and reaching around to wash your back must be avoided during your initial recovery period. With that in mind, you may want to stock up on dry shampoo or have a close friend or your caretaker help you with bathing. You’ll likely be restricted to sponge baths until your surgeon gives the green light to step into the shower. When showering, it is important to face away from the water spray and carefully dry incisions if they get wet.
- Light exercise: You can forget the gym for a few weeks. Lifting arms above your head and objects heavier than five pounds is generally not allowed for two weeks. However, general movement is encouraged to promote circulation.
- New bras: After your surgery, you will have to wait four to six weeks until you can trade the sports bra for new lingerie. In the meantime, make sure your sports bras provide sufficient support and do not rub your incisions.

RELATED: Drop and Fluff — A Breast Augmentation Recovery Timeline
Breast Implant Scars
One of the most pressing concerns for women undergoing breast augmentation is the scar it leaves behind. Every person heals differently because wound repair depends on a number of factors, such as age, skin tone and complexion, and incision location and size.
- Age: Younger skin heals better because of higher collagen production. But as we age, collagen production slows down and skin becomes thinner and less elastic. There are some things that you can do to increase collagen production, such as red light LED and topical retinoid creams.
- Skin tone: Some skin colorations are more likely to scar than others. Those with darker skin tones are more likely to form hypertrophic and keloid scars, which are characterized by an overgrowth of scar tissue. However, some scars tend to blend in better with darker skin while people with fairer skin may find that their scars are more noticeable.
- Size and depth of the incision: The larger the incision, the longer it will take to heal. And the longer it takes to heal the wound, the higher the risk of infection or scarring occurring.
7 Tips to Minimize Scars and Promote Healing
- Stop smoking: Nicotine and other chemicals found in cigarettes and other forms of tobacco suppresses the immune system, constrict blood vessels, and slow the flow of hemoglobin and oxygen — important wound healing molecules — which can impact on the skin as it heals.
- Stop drinking: Alcohol thins the blood and interferes with the clotting required to close and heal an incision. Another side effect of alcohol is that it slows the collagen production needed to mend the incision, and also lowers the body’s immune response to bacteria, which can lead to infections.
- Improve your diet: Proteins, fatty acids, vitamins, and minerals play a role in wound healing by speeding tissue repair. To protect your cosmetic investment, make sure your post-surgical diet includes those “powerhouse” foods such as leafy greens, wild salmon, and nuts. You’ll also be asked to reduce sodium intake to prevent bloating, which can put pressure on your incisions. Another tip: set a daily reminder to take your multi-vitamins.
- Stay hydrated: Water makes up 2/3 of the human body, and not drinking enough of it can throw the body out of balance, slow the flow of oxygen, minerals, and nutrients to the wound, and render the skin more fragile and prone to bacterial infection. Post surgery, aim for 3 liters of water for day.
- Get enough sleep: Sleep helps the body produce more infection-fighting white blood cells and triggers the hormones that encourage tissue growth.
- Stay out of the sun: UV rays are bad for the skin in general, and are even worse for scar tissue. Newly formed tissue is extremely sensitive to sun exposure, and excess UV rays can lead to the darkening and thickening of the newly formed scar. The recommended time to avoid the sun ranges from six months to a year. If it’s not possible to avoid ultraviolet rays, use SPF 30, clothing, or silicone tape to cover the scar.
- Minimize activity: Tension on wounds can undo the careful sutures your surgeon placed, and this pressure on a newly closed incision can cause widening or hypertrophy of the scar. For this reason, it’s important to follow doctor’s orders by having someone with you for 24 hours post surgery to ensure you don’t put tension on your scars by reaching for something or stretching your arms. For two to four weeks post surgery, avoid or restrict lifting your arms above your head, bending down, or lifting heavy objects.
Effective Scar Treatment Options
As soon as the surgical dressings come off and the incisions are sealed, you can use one or more techniques to try to reduce the appearance of scars.
- Silicone sheets: These 100% silicone wound enclosures cover the incision, keeping the wound hydrated and soft and creating an optimal environment for healing. Another benefit of these medical grade adhesives is that the sheets help stabilize the incision and alleviate tension on the skin, which can prevent the widening of scar and keloids from forming. Silicone sheets are worn for at least 12 hours of the day, and are recommended for postsurgical recovery for two to 12 months.
- Silicone gel: Topical gel made from silicone can be used to promote healing by keeping the wound hydrated, soft, and free of bacteria. The gel is painted over the scar a few times per day, and it dries to form a transparent bandage over the wound.
- Laser and light therapy: Laser skin resurfacing is used to reduce wrinkles on the face, but it can also be used to reduce the appearance of scars, especially hypertrophic or keloid scars. However, darker skin tones may not respond well to certain types of lasers. In these cases, red light LED can be used instead.
- Microneedling: This anti-aging technique is most commonly used for facial rejuvenation, but it can also be used to fade scars. Micro-thin needles create thousands of tiny vertical incisions on the face to stimulate the production of collagen. As these tiny micro-channels fill with collagen, the newly formed skin can dilute the appearance of scars and flatten raised scars.
- Cortisone injections: In some cases, surgeons may inject steroids directly into an incision to help decrease redness, burning, or itching of the scar, and flatten keloid and hypertrophic scars.
RELATED: Minimizing and Treating the Appearance of Surgical Scars
Breast Augmentation Risks and Complications
Breast augmentation, like any surgery, comes with risks that can be minor — or they can be life-altering. The most significant risks do not necessarily take place during the surgery, but may occur months or even years after you leave the operating table.
- Displacement: Implants may shift from their placement and may bottom out, become misaligned, rupture, or appear deformed. Surgical revision is needed to reposition the implant.
- Rupture: According to the FDA, 10 percent of implants rupture within the first five years. Some of the causes of rupture include overfilling saline implants and subsequent trauma to the chest. However, the silicone shell of the implant will degrade in the body over time, and holes may form through which the saline fluid or silicone gel can escape.
- Capsular contracture: Capsular contracture is one of the serious risks of breast augmentation. The scar tissue that naturally forms around an implant to keep it in place may harden and thicken. When this occurs, the thickened tissue may make breasts feel abnormally hard, distort their appearance, and cause some pain or discomfort from the tightening of the capsule. The seriousness of capsular contracture is rated in four grades, and grades three and four may require revision surgery. It is not possible to predict if it will happen or when, but some studies suggest that bacterial infection may contribute to contraction. To avoid this, doctors will prescribe a round of oral antibiotics to reduce the risk of infection after surgery. It is vital to take the entire course of antibiotics. Some will also prescribe a leukotriene inhibitor that has been shown to prevent or reduce the severity of capsular contraction, and in some cases even reverse it.
- Infection: Infection is a rare but serious complication that can derail your breast augmentation. Bacteria can cause inflammation that increases the chances of capsular contracture, or even requires removal of the implants for weeks or even months to allow the body to heal before they can be refitted. For this reason, plastic surgeons will prescribe a round of antibiotics to avoid the risk of infection while healing. You should practice good hygiene and follow postoperative activity restrictions. Patients and their caretakers should handle surgical drains (if present) with extreme care and wash their hands frequently to avoid possible infection. Also avoid environments with high levels of bacteria, such as gyms, saunas, and hot tubs.

RELATED: Is Breast Implant Illness Real?
Latest Techniques and Scientific Studies
As one of the most popular cosmetic procedures, breast augmentation is constantly scrutinized by surgeons who seek more effective methods of performing surgery. While breast augmentation is safer than ever before and offers results that leave patients highly satisfied, there is always room for further improvement.
One of the most exciting new advances currently being investigated is breast tissue engineering. A study published in Tissue Engineering journal in 2017 reported that breast tissue engineering offers a novel and innovative approach to providing a safe, natural material to augment the breasts. Current augmentation materials are characterized by inherent limitations: silicone implants can sometimes cause complications such as capsular contracture, requiring removal or revision surgery, and lipofilling of the breast using fat can result in significant volume loss.
Breast tissue engineering is based on the premise of creating a “scaffold” for augmentation with the patient’s own stem cells to generate autologous new breast tissue. Stem cell surgery is widely acknowledged as one of the most promising new paradigms of medical and surgical practice in the 21st century. The study also discusses the potential of combining tissue engineering with lipofilling. However, at present, breast tissue engineering is still in its incipient phases.
Another compelling development that has also arisen in response to capsular contraction is experimentation with lining implant surfaces with biomimetic breast tissue. A 2017 study outlines the potential of using silicone implant surfaces textured with biocompatible materials to improve the performance of the implant once inserted. These implants reduce postoperative inflammation and result in a more successful integration of the implant into the body.
Frequently Asked Questions
Do implants cause cancer?
Extensive studies have been conducted and none have shown that silicone breast implants cause cancer. However, silicone implants may make it harder to detect tumors during mammogram, which can delay cancer diagnosis. Women with breast implants have a very low but increased risk of developing a rare type of cancer called anaplastic large cell lymphoma (ALCL) in the breast tissue surrounding the implant, but this is not breast cancer.
Will a breast augmentation interfere with breastfeeding?
Between 1% to 5% of women who have never had breast implants are unable to breastfeed their children, and there is no way to know in advance if you fall within this statistic until you have given birth and attempted to breastfeed. Typically, breast implants do not interfere with breastfeeding, and most women are able to breastfeed after surgery. However, women who have undergone a mastectomy may not be able to breastfeed due to extensive loss of breast glands and tissue.
Am I too young for breast augmentation?
The FDA has approved implants safe for use in patients 18 years old and older, and women under the age of 22 are restricted to saline implants. However, there is no legal minimum age to get breast implants. 7,840 young women between the ages of 13 and 19 received implants in 2015, according to the American Society of Plastic Surgeons (ASPS), and 3,429 women under the age of 18 underwent the procedure in 2015, according to the ASAPS.
Most doctors will recommend women to wait until they have achieved a stable weight and understand that their body will change during and after pregnancy.
How much will it cost?
Breast augmentation surgery costs vary depending on the region where you undergo surgery, the type of implants used, and whether or not a breast lift is also performed.
The average cost for saline implants is $3,268, and $3,618 for silicone implants, according to the American Society of Aesthetic Plastic Surgeons.
Many offices offer financing or will let you pay by credit card. However, you should keep in mind that breast implants aren’t a one-time investment and you will need to budget extra cash to pay for routine check ups or MRIs to monitor the health of your implants. You will also be responsible for any additional surgical fees for revisions, complications, or replacement implants after the warranty expires.
How much will it hurt?
According to a survey conducted by the ASPS, women reported an average pain score during recovery of 5.9 out of a 10-point scale.
What are the risks?
As with any surgery, there are risks and side effects of breast augmentation. If you are undergoing general anesthesia, risks include nausea and pulmonary complications, rupture, displacement, capsular contracture, and infection.
How long do implants last?
Undergoing a breast augmentation is likely to be the first of several surgeries to maintain your implants. Implants have an average lifespan of 10 years — although many last several years longer — and need to be monitored regularly to ensure their integrity and check for leaks. It’s likely that one or both will need to be replaced over your lifetime, and many women decide to change sizes down the line.
How long will it take to recover?
The surgery takes 1-2 hours. Most women are back to work within 1-2 weeks, and patients reported that they felt “back to normal” about 25 days after surgery.
How do I pick the right size?
Limited evidence suggests that tissue-based planning systems — using clinical guidelines to determine the optimal breast implant dimensions for individual patients – appear superior to other approaches such as dimensional analysis or patient or surgeon preference.
How long will swelling last?
Most swelling will subside within four to six weeks.
When can I start exercising?
Lifting arms above your head and objects heavier than five pounds is generally not allowed for two weeks. However, general movement is encouraged to promote circulation.
When will my breasts “fall”?
Breasts will settle into position and soften between three and six months.
What bras should I wear after surgery?
Plastic surgeons have varying opinions on the types of bra to wear after surgery, and you should discuss your concerns about proper support with your doctor. If implants were inserted along the breast fold, you should avoid any bra with underwire until the scars are healed to avoid irritating the stitches.
What are the revision rates?
Between 25-30 percent of women experience capsular contracture, which almost always requires surgery to correct. As many as 20 percent of women need to have their breast implants removed within 8 to 10 years, according to the FDA.
How long will I need to take off from work?
On average, women used prescription pain medication for five days and were off work seven days, according to a survey by ASPS.
Breast Implant Statistics
- The average breast augmentation patient age is 34 years old.
- 7,840 women between the ages of 13 and 19 received implants in 2015.
- 15 percent of women opted for saline implants, and 85 percent chose silicone.
- 88 percent of silicon implants used were round, 12 percent of silicone implants were shaped.
- The average implant volume is 390 cc.
- 18,135 women used their own fat to augment their breasts in 2015.
- 38,071 had their implants removed, either to change the implant size or for other personal or medical reasons.
- 92 percent of women reported improved self-esteem after breast augmentation.
- 64 percent reported an improved quality of life.
- Nearly 40 percent of the women surveyed experienced at least temporary nipple numbness after surgery.
- Persistent numbness was reported by only two percent.
- Hypertrophic scarring occurs in 2 – 5 percent of patients.
- Hematomas – pockets of blood – may form in the incision of 1- 6 percent of patients.
- Infection (cellulitis) occurs in 2 – 4 percent of patients.
- $3,497: national average cost for saline implants.
- $3,964: national average cost for silicone implants.