- We now know there’s a genetic component to developing carpal tunnel syndrome.
- If your case is bad enough, surgery may be your only option.
- The most reliable treatment is known as carpal tunnel release.
- Recovery time from this procedure is long but worth it.
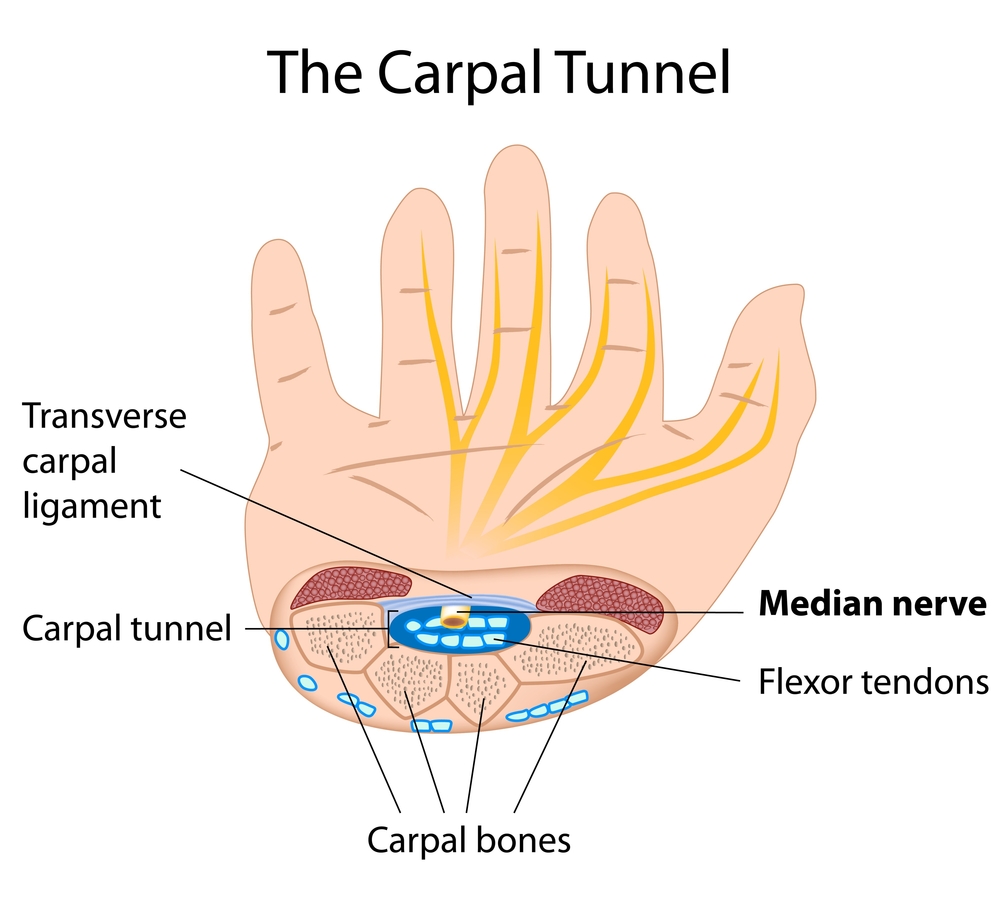
What is the carpal tunnel?
The carpal tunnel is a physical space in your wrist that runs between the wrist bones at the bottom and the transverse carpal ligament at the top. This space allows the median nerve and the tendons that help your fingers move to pass through unimpeded. It’s an actual tunnel through which essential working parts of your hand pass.
Still not clear? Hold your arm out with your wrist facing up. Do you see the tendons running from your wrist to your hand beneath the surface of your skin? They seem to disappear right where your hand and wrist meet. This is the location of the transverse carpal ligament. Beneath that is the carpal tunnel.
What is carpal tunnel syndrome?
Sometimes, due to repetitive motion injury, this tunnel becomes contracted. It swells, pinching the median nerve and the tendons, which causes chronic pain and ultimately leads to decreased mobility. This is carpal tunnel syndrome.
While there are many ways of treating carpal tunnel syndrome, the most reliable procedure involves expanding that tunnel in a surgical process known as carpal tunnel release surgery. When is it time to consider carpal tunnel release? And what should you expect from the procedure?
What is carpal tunnel release surgery?
Also known as carpal tunnel decompression surgery, carpal tunnel release involves cutting the transverse carpal ligament. In doing so, the tunnel expands and any pressure placed on nerves and tendons is released. When describing this process to his patients, Dr. David C Hay, an orthopedic surgeon with the Cedars-Sinai Kerlan-Jobe Institute in Los Angeles, refers to the ligament as a “tight belt.” When the belt is cut, the pants get looser and the body is more comfortable. It’s that simple.
But why should this be necessary to begin with? Shouldn’t there be a way to decrease pressure within the carpal tunnel without surgery? There are in fact several non-surgical solutions available, but they may not be effective enough to give long-term comfort.
Medical professionals used to think that carpal tunnel syndrome was exclusively caused by overworking the wrist, especially with repetitive motions like typing. But they’ve since learned that there is a genetic element to the condition. Some people are born with smaller carpal tunnels than others, leaving them predisposed to developing the condition and making a non-surgical solution more difficult to find.
What’s more, untreated carpal tunnel syndrome can lead to serious quality of life issues and other complications. In time, your fingers fingers and thumb could become weak and, in extreme cases, virtually unusable. In short, the longer you wait to find a lasting solution, the more pain and frustration you can expect.
How is carpal tunnel syndrome diagnosed?
You’ll need a confirmed diagnosis of carpal tunnel syndrome before surgery. There are a number of ways to test for the condition. These are the three most common:
- Compression Test – Your wrist is squeezed to further compress the median nerve. If this causes symptoms to flare up, then you have carpal tunnel syndrome.
- Phalen’s Test – This test, which involves hyperflexing the wrist for about a minute, is also intended to trigger symptoms.
- Tinel’s Test – In this test your doctor will tap on the inside of your wrist above the carpal tunnel. If you feel something like an electric shock, then you have carpal tunnel syndrome.
Sometimes, the above tests aren’t conclusive enough. In these cases, surgeons may run more advanced tests, including electromyography (EMG) or electroneurography (ENG), both of which read the electroactivity of the median nerve to determine if it’s actually being compressed.
Do I need carpal tunnel release surgery?
Although carpal tunnel release is demonstrably effective, and addressing carpal tunnel syndrome head on is definitely important, that shouldn’t scare you away from non-surgical options. Your physician will likely expect you to try several non-surgical options before recommending surgery, including any of the following:
- Pain and anti-inflammatory medications (NSAIDs)
- Physical therapy
- Wrist splints
- Corticosteroid injections
- Ergonomic changes to equipment at home or work that may be causing the problem
Of course, whether or not your surgeon recommends these options depends on the extent of your symptoms. Dr. Hay distinguishes between sensory symptoms and motor symptoms. The former are centered largely on pain and related tingling and can be persistent or intermittent. The latter are more severe and involve loss of muscle function.
Surgery should be recommended for those with persistent sensory symptoms and especially recommended for those with motor symptoms. In the latter case, Dr. Hay urges, “You’ve got to have the surgery – it’s almost too late.”
» Want to know if you’re a good candidate for surgery? Meet our medical review team.
How do I prepare for carpal tunnel release surgery?
Start by finding the right surgeon. Your regular doctor will probably refer you to a specialist. But if you find yourself shopping around, look for a plastic surgeon, orthopedic surgeon, or even a neurosurgeon. In particular, focus on surgeons that have extensive experience working with hands or specifically with treating patients who have carpal tunnel syndrome.
Once you’ve locked down a doctor and scheduled a date for surgery, you’ll be given some instructions on how to prepare for the big day. You’ll likely have some pre-surgery appointments during which you’ll undergo routine preliminary tests such as blood tests and an EKG. You’ll also be expected to fast for six to twelve hours prior to the procedure.
Finally, there are things you can do at home to ready yourself for the recovery process. You will need to limit movement in the affected hand. If you live alone or expect to be alone for long periods of time, then prepare some microwavable meals and turn on voice commands for your electronics if possible. You’ll also want to make sure you won’t need to go shopping for awhile.
How does carpal tunnel release surgery work?
There are a handful of methods for performing carpal tunnel release surgery, but they all involve cutting that same transverse carpal ligament.
When you go in for your procedure, you’ll lay back while your surgeon sterilizes your wrist and hand. During this time, the surgeon may use a tourniquet to reduce blood flow, although many surgeons deem this unnecessary. In rare cases, you may receive general anesthesia, putting you to sleep for the duration of the procedure. Most patients receive local anesthesia, sometimes accompanied by a sedative.
Once the anesthesia takes affect, your surgeon will perform the surgery in one of several ways:
Open Carpal Tunnel Release
The surgeon makes an incision from the wrist to the bottom of the palm, exposing the transverse carpal ligament and then cutting it with a scalpel. Sometimes, tissue around the median nerve is also removed. In extended open release, the classic form of the procedure, the incision is two inches long. More recently, surgeons like Dr. Hay himself have started performing a “mini” open release procedure with an incision smaller than one inch.
Endoscopic Carpal Tunnel Release
This version of the procedure leaves the body less exposed. It involves two half inch incisions, one on the wrist and one on the palm. A camera is inserted through one incision and surgical tools are inserted through the other. This form of the surgery is said to heal faster than does open carpal tunnel release. Similarly, endoscopic carpal tunnel release has a few variations, including one which requires only a single incision.
Carpal Tunnel Thread Release
In this procedure, the surgeon doesn’t use a scalpel to sever the ligament. Instead, they insert a needle into the hand using ultrasound technology as a guide. The needle is used to loop a thread around the ligament that then gently severs it. This method is thought to result in minimal scarring. However, this newer procedure is riskier and not yet widely practiced, since doctors aren’t able to see what they’re doing quite as well. Dr. Hay questions if the benefits are worth the risk, given the imprecise nature of the procedure. “There’s a lot going on in the carpal tunnel, so any of these blind procedures where you’re doing it through a needle and ultrasound – there’s just a risk of a problem,” he says, noting that there’s no reason to change a procedure that is already safe and has high patient satisfaction.
In nearly all cases, surgeons perform either open carpal tunnel release or endoscopic carpal tunnel release. Once the surgery is completed, your surgeon will suture the wound closed and dress your wrist with a bandage or a splint.
» Curious about different methods for carpal tunnel release? Ask a doctor on our forum for more information.
What is recovery like?
Recovery from a carpal tunnel release is not quick. It can take several weeks to months for your hand to fully heal. The longer you suffered from carpal tunnel syndrome, the longer your recovery will likely be.
When you first go home after surgery you’ll be given painkillers, a wrist splint or dressings, and further instructions. Some surgeons will have you wear your dressings or splint for 1–2 weeks and then have them removed at a follow-up appointment. Others, like Dr. Hay, only require you to wear them for 3–4 days. Your surgeon may also instruct you to elevate your hand at night. This helps fluid drain from the surgical site and prevents painful swelling.
During this time, you’ll need to limit movement of the affected hand. That means no driving for at least a few days after surgery, no writing for about a week, and no pulling, gripping, or pinching for around 6–8 weeks. Your recovery will be helped along by physical therapy, which you’ll begin after your wrist splint or dressings are removed.
What are the risks and complications?
For the most part, carpal tunnel release surgery is very safe. A little pain, bleeding, and minor swelling are all normal parts of having had surgery. Generally, they’re nothing to worry about. There are however some times when you might want to call your surgeon:
Infection
Keep an eye out for signs of infection. Redness and swelling fall under this category, but they might also be completely normal. Look for them in conjunction with other symptoms of infection like purulent (pus-like) discharge, renewed bleeding or pain around the incision, and persistent fever.
Pillar pain
In some cases, patients may experience “pillar pain” at the incision site. Dr. Hay uses the metaphor of a work boot to describe this phenomena. “If you step on it, you can’t feel the sole,” he says. “But if you cut the sole, you can feel those two thick edges.” This is the case with the transverse carpal ligament before and after it’s been cut. Pillar pain usually goes away with time and physical therapy.
Nerve and blood vessel damage
Finally, rare but possible complications from the procedure itself include damage to the median nerve, any of the nerves branching from it, or surrounding blood vessels. If nerves are damaged, you could experience new or renewed pain and will likely need a second surgery. Damage to the median nerve could also result in a painful neuroma, or “pinched nerve.”
According to Dr. Hay, such damage is rare and will more than likely not happen. But if it does, then it can be difficult to repair. When it comes to nerve repair, haste is important. Unfortunately, nerve damage symptoms may not be obvious until it’s too late for an effective second surgery.
How well does carpal tunnel release surgery work?
The prognosis for carpal tunnel release is very good. Many people report a complete reversal of symptoms, noting that they feel cured. On the other hand, some people do experience ongoing pain and numbness after surgery.
Overall, most people find carpal tunnel release to be beneficial. In fact, approximately 75 to 90 out of 100 patients report that their symptoms improved after surgery. This includes decreased pain and numbness as well as increased muscle strength.
Dr. Hay encourages people to explore the surgical option. He performs five or more surgeries a week and cites his success rate at over 90%. “It’s a reliable, common, predictable procedure,” he says. “Patients shouldn’t be afraid of carpal tunnel release.”
What is the cost of carpal tunnel release surgery?
The surgery takes about 15 minutes to perform and should be covered by insurance. If you do not have insurance, the surgery will cost $2,000-$2,500.
» If you think you might have carpal tunnel syndrome and want to discuss surgical options, meet our medical review team.