- A dead or non-vital tooth is one which has no access to a fresh supply of blood.
- Tooth decay and trauma are the most common causes of dead teeth.
- Dentists diagnose dead teeth by taking x-rays and testing the tooth for sensitivity to heat, cold, and electrical stimuli.
- Dentists can treat dead of dying teeth by performing root canals or extractions.
Your smile is an important asset; a beautiful smile, with rows of straight, white teeth projects friendliness and confidence. But what if one your teeth is a different color than the rest, or worse, is causing you pain? If this is the case, you may have a dead tooth.
If you suspect you have a dying or dead tooth, you should schedule a visit with your dentist as soon as possible. In many instances, he or she will be able to treat the tooth and save it.
What is a dead tooth?
A dead or non-vital tooth is one which no longer has access to a fresh blood supply from the vessels in its root.
Teeth are living structures, comprised of two outer layers: the enamel and the dentin, plus an inner layer called the pulp or nerve. Whenever the blood flow going to the pulp becomes restricted or cut off — by trauma or infection, for example — the pulp can die.
A dead tooth may appear darker or a different color than the surrounding teeth due to the body’s inflammatory response, which sends more red blood cells into the tooth in an attempt to repair the damage.
A tooth can die within a few hours or slowly over the course of months or years, depending on what is causing the blood supply restriction.
What causes a dead tooth?
There are two main causes: dental decay and trauma. While you might not always be able to prevent dental trauma, you can reduce your chances of experiencing tooth decay by practicing good oral hygiene and avoiding foods that exacerbate tooth decay, such as those containing high amounts of processed sugars.
Cavities
According to the Centers for Disease Control (CDC), 18.6 percent of American children from the ages of 5 to 19 years, and 31.6 percent of Americans aged between 20 and 44 years have untreated dental caries (cavities).
Tooth decay can cause a tooth to die when cavities penetrate the enamel and dentin, inviting bacteria and other microorganisms into the inner layer of the tooth (dental pulp) where they colonize it. The tooth then becomes infected, which cuts off its blood supply.
Trauma
Sports injuries or other trauma are another common cause of dead or dying teeth. If a ball hits you in the mouth, for example, or you land on your face after a tackle, one or more of your teeth can become loose or cracked. If you play contact sports, wearing a mouth guard can help to protect your teeth from damage.
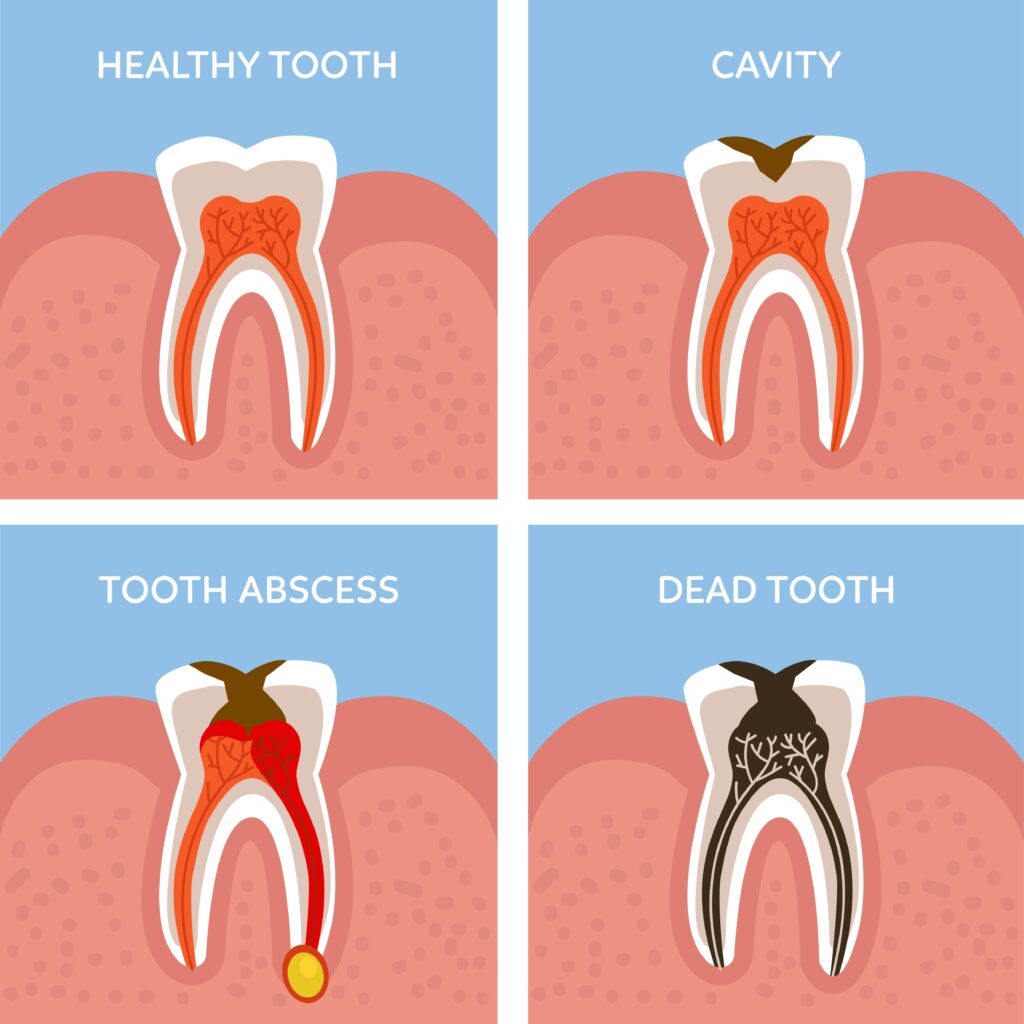
How do I know if my tooth is dead?
You might suspect you have a dead tooth should you notice that it is noticeably darker or a different color than the rest of your teeth. A variation of color from one tooth to the others is the key: teeth stained from regular coffee drinking, for example, will be uniformly yellowish, while a dead tooth is likely to be a markedly different color than the surrounding teeth.
Pain from a dying or infected tooth can be incredibly intense, and provides a clear sign that the problem needs to be addressed. The dying nerve may make your tooth extremely sensitive to hot or cold foods. Infection may also cause severe pain.
Until you are able to see your dentist, take over-the-counter anti-inflammatory medications such as acetaminophen and ibuprofen. You should also avoid hot and cold foods or drinks.
Does a dead tooth always hurt?
No, a dead tooth does not always cause pain. It may only hurt as the nerve dies, or if the tooth becomes infected.
In some cases, the tooth will stop hurting after the nerve has died. However, you may continue to feel pain if an infection or something else puts pressure on the layer of tissue and nerves tissue that surrounds the tooth, also known as the periodontal membrane.
Can a dead tooth cause bad breath?
On its own, a dead tooth is unlikely to cause bad breath. If you have bad breath, this could be a sign that your tooth is infected.
If you have a bacterial infection, you may experience some of the following symptoms as well:
- Intense pain
- A bad taste in the mouth
- Swollen gums around the infected tooth
- A pimple (dental abscess) in the gum tissue
How is a dead tooth diagnosed?
Your dentist can diagnose a dead tooth by learning about your symptoms and testing its response to hot and cold or electrical stimuli. X-rays of your mouth and jaw may also be performed.
What are the treatment options for a dead tooth?
Depending on the amount of damage to the enamel and the severity of the infection, your dentist can save your tooth by performing an endodontic (from the Greek, literally meaning inside the tooth) procedure called a root canal. If there’s not enough tooth left to save, he or she may extract the tooth instead.
Root canal
A root canal is a procedure during which a dentist removes the damaged or infected pulp from your tooth, and shapes the root with special instruments. He or she then fills the space and seals it. If your tooth requires a crown, you will need to return to the dentist’s office for fitting and application.
Not every tooth needs a crown after root canal surgery. If your own tooth doesn’t need one but you’re concerned by the discoloration, your dentist can apply veneers or use dental bleach to lighten the enamel.
If your tooth needs a crown, you shouldn’t bite or chew with it until it has been placed. Otherwise, you could crack or damage the tooth.
Extraction
When the tooth is far too damaged to be saved, there are two types of extractions that can be performed — simple and surgical extractions.
Simple extractions can be done without surgery using forceps and elevators. Surgical extractions involve cutting into the gum tissue or removing the tooth in pieces rather than as a whole.
Your dentist will decide which type is indicated in your case, but in general, dentists use the simple method when there is enough exposed tooth above the gums to grab, and the surgical method when the tooth has broken or decayed to the point that most of its surface is under the gum.
Dentists may also choose the surgical method when dealing with teeth that have curving roots or other structural problems that make simple extraction impractical.
Will a dead tooth fall out?
While a dead tooth may eventually fall out given enough time, it’s never a good idea to wait for this to happen. The chances are high that it will become infected long before it falls out, and a dental infection can be life-threatening when it moves into the bloodstream.
Can a dead tooth actually kill you?
A dead tooth by itself will not make you sick or kill you. However, if it gets infected and that infection spreads into your bloodstream, you can become very ill, and your condition could quickly become life-threatening.
If you have any of the following symptoms, immediately seek medical help:
- A fever higher of over 103 F
- Difficulty breathing
- Severe facial swelling (cellulitis)
- Severe headache
- Stiff neck
Will a dead tooth go black?
A dead tooth can blacken, but it can also turn yellow, grayish, or brown. A dead tooth changes color because of the body’s inflammatory response, which brings more red blood cells into the tooth’s pulp and stains the enamel.
Can a dead tooth be whitened?
If your dead tooth does not need a crown following a root canal, options for whitening or lightening the discoloration include bleaching and veneers.
Can a dead tooth be saved?
Yes. As long as there is enough tooth structure there to save and the infection isn’t too severe, your dentist can perform a root canal to save your tooth.
How can I avoid getting a dead tooth?
You can lessen the risk of developing a dead tooth by fighting tooth decay with proper oral hygiene, and protecting your mouth from injury should you play contact sports.
Take care of your teeth by doing the following:
- Brush them twice a day.
- Floss once a day.
- Drink plenty of water between brushings, as it flushes away the bacteria and sugars that cause tooth decay.
- Avoid foods that contain a lot of processed sugars.
- See your dentist twice a year for dental check-ups.
Wear a helmet and a mouth guard if you play contact sports like hockey, football, or boxing. A mouth guard protects your teeth from impacts, such as getting hit with a ball or falling on your face.









